


An age-related disease that compromises your most critical vision responds to a promising new therapy
I Can See Clearly Now

Dorothy Beimfohr, AMD patient.

The treatment is easy, quick and painless. The trick is to catch patients when they are just beginning to lose vision, since those who have had the disease for years and have formed retinal scar tissue will not benefit from any currently available treatment.
![]()
For an older adult like Dorothy Beimfohr, who loves to read and needs to drive, age-related macular degeneration (AMD) is a terrifying diagnosis. “When I first heard that, it really just shook me,” she says. How would this eye disease—in which abnormal blood vessels creep under the center of the retina, leaking blood and destroying vision—change her life? Would it curtail her pleasant visits to the Mascoutah, Illinois library? Would it rob her of the sight of her five grandchildren?
“When patients lose their center of vision, you can't tell by looking at them that they are handicapped,” says Nancy M. Holekamp, MD, assistant professor of clinical ophthalmology, who treated Beimfohr. “But they won't recognize you because they can't see your face, they have a hard time dialing your phone number and if you ask them to read something, they can't. Consequently, they lose a lot of their independence.”
This disease, the leading cause of blindness in people 65 and older, is not only devastating for patients—it also is frustrating for their physicians. AMD sufferers, who otherwise may be in perfect health, become so desperate that they sometimes resort to sham treatments in an attempt to find a cure. And ophthalmologists, armed with few clinical weapons to fight the disease, have little they can do to help.
At the Barnes Retina Institute (BRI), a national leader in retinal research, Washington University faculty members are involved in several clinical trials that are testing new therapies aimed at saving or restoring vision in AMD patients. In fact, BRI faculty members have participated in most of the major trials that have taken place over the past several decades. A recent trial that examined a new approach to treating AMD, photodynamic therapy, has shown promising results.
Searching for effective treatment
“We see thousands of patients a year with macular degeneration; they make up at least 25 percent of our caseload,” says M. Gilbert Grand, MD, professor of clinical ophthalmology. “This is a very significant problem, and we are continuing to see more of it as the population ages. Among the saddest aspects has been having to tell patients that we have limited forms of treatment.”
In the late 1980s and early 1990s, Washington University and other institutions participated in the Macular Photocoagulation Study, sponsored by the National Institutes of Health, which targeted patients with wet AMD. The first phase of this trial focused on patients whose blood vessels had penetrated the macula but had not yet reached the fovea, its tiny, 500-micron-wide center.
In the study group, clinicians used a conventional, thermal laser to destroy the vessels; in the control group, patients did not receive laser treatment. The results showed that laser therapy was effective, but it was not a perfect solution. Nearly 50 percent of the time the vessels grew backand the laser was destructive, creating a blind spot where it did its work.
Still, the results were positive enough that researchers went further, studying patients whose blood vessels had grown into the fovea. The laser treatment again yielded mixed results. It destroyed the blood vessels and stymied their regrowth, but it also destroyed the center of vision, rendering patients legally blind. Even so, 18 months after treatment, the treated patients were better off than the untreated control group.
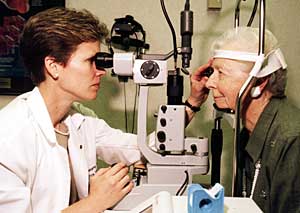
Nancy M. Holekamp, MD, examines the eye of patient Sametta House.
About the same time, two Washington University ophthalmologistsMatthew A. Thomas, MD, of the BRI, and former department head Henry J. Kaplan, MDpioneered an extraordinary form of surgery in which they elevated or focally detached the retina, plucked out the errant blood vessels, and then put the retina back in place. A multicenter clinical trial currently in progress, with Thomas as national vice chairman, is evaluating the success of this surgery, but it appears so far that it works best in younger patients.
Other trials are ongoing. A national, NIH-sponsored studythe Complications of AMD Prevention Trial (CAPT)with Grand as principal investigator, is studying the use of low-power laser to treat dry AMD, which can be a precursor to the wet form of the disease.
BRI physicians also are participating in a study of macular translocation surgery, developed at Johns Hopkins. And they are enrolling patients in a trial sponsored by Alcon Research, Ltd., to see whether a new compound, anecortave acetate, stops the leakage from these abnormal blood vessels.
Photodynamic therapy may be one answer
But the latest and most promising form of AMD treatment is the photodynamic therapy (PDT) that Dorothy Beimfohr underwent, in which a non-thermal laser targets leaky blood vessels.
Washington University participated in the clinical trials of PDT, which was approved by the FDA in April 2000 for one form of AMD. Already, BRI physicians use it daily, and that usage may soon increase, since the FDA is on the verge of approving its use in other forms of AMD. In addition, PDT has strong potential for treating patients with other retinal diseases.
Beimfohr is delighted with the outcome of her PDT treatment. While many patients have bilateral disease, her left eye has not been affected. But the vision in her diseased right eye has improved from 20-80 to 20-40enabling her to drive once again.
“PDT is an ingenious idea,” says Holekamp. “The eye is set up perfectly for this type of novel therapy. And it only destroys the abnormal blood vessels without hurting the retina, which is a huge advantage.”
The treatment is easy, quick and painless. The trick is to catch patients when they are just beginning to lose vision, since those who have had the disease for years and have formed retinal scar tissue will not benefit from any currently available treatment.
Retina specialists initially perform a fluorescein angiogram test to determine which patients are eligible for PDT treatment.
When Beimfohr came in for her PDT treatment, she received a 10-minute infusion of photoporphyrin dye, Visudyne™, into a vein in her arm. The dye coursed through all the blood vessels in her body, including the abnormal vessels in her retina. Then Holekamp shone the non-destructive laser at her eye for 83 seconds. Throughout the procedure, Beimfohr was fully awake; afterwards, she only had to avoid direct sunlight for five days.
Following treatment, ophthalmologists retest PDT-treated patients at three-month intervals to determine whether any regrowth has occurred. If it has, they repeat the treatment.
Beimfohr was fortunatenot only did the photodynamic therapy prevent the abnormal blood vessels from returning, her vision actually improved.
In the clinical trial of PDT, 67 percent of patients who received the treatment were stabilized or improved by it. Only 16 percent, however, had a return of good vision.
“So it is not the cure that we were hoping for,”
says Holekamp, “but it is something else that we have to offer patients
who otherwise have no hope.” ![]()
|
WHEN THE CENTER OF SIGHT FAILS The center of the retina, called the macula, is highly detail-sensitive, allowing you to read the page of a book or recognize your friend's face. Macular degeneration attacks this critical area of vision. “Dry” AMD AMD comes in two basic forms. The “dry” type is characterized by spots called drusen and sometimes by atrophy of the tissue layer that underlies the retina. No treatment exists for dry AMD, but it is also a milder, more slowly progressive disease that only accounts for 10 percent of severe vision loss among AMD patients. “Wet” AMD The story is much different with the second, “wet” form of the disease, in which blood and fluid from abnormal blood vessels leak onto sensitive photoreceptors in the macula. Among AMD patients, this type of the disease accounts for 90 percent of all severe vision loss. Often, this change occurs suddenly, without warning. It is not yet known exactly why this happens. Attempts to link AMD to smoking or diet have not been successful. It is rare in Asian and African-American patients and most common in women 60 and older of Scandinavian descent. There may be a hereditary component to the diseasebut what stands out is its correlation with age. The longer you live, the more likely you are to develop it. |