


Look who’s talking
A pioneering surgery makes the news—and changes a life.

“I refused to believe that I had to spend my life like that,” Amy Hancock says of being speechless.



“It was not a routine procedure exactly, but it went very smoothly— as well as I could possibly have hoped.”
RANDAL C.
PANIELLO, MD


![]()
IN AN AGE OF SENSATIONAL NEWS AND “REALITY TV,” the true story of a pioneering surgery has risen above the fray, making St. Louisan Amy Hancock an “overnight” media celebrity. A complex procedure restored her ability to speak—the first of its kind performed in the U.S.—and its successful outcome has grabbed local headlines and spurred national television coverage. “This can’t last, but for now I am having the time of my life,” says Amy happily, in her raspy but confident new voice.
It was not a transplant, not an artificial device, but a reconstruction of Amy’s voicebox performed on May 23 at Barnes-Jewish Hospital by head and neck surgeon Randal C. Paniello, MD, that revived Amy’s ability to speak. No more robotic-style speech from holding an electrolarynx device to her throat—as she had done for five years since losing her own larynx to cancer.
Best of all, Amy says, her experience and the accompanying publicity may help others achieve the same satisfying result. While her operation was still in progress, an e-mail reached Paniello’s office from a man who had heard the news and hoped that voicebox reconstruction might also benefit him. “That’s the kind of thing that really makes this all worthwhile,” she says.

A production crew for the Discovery Health Channel interviews Amy Hancock at the Missouri Botanical Garden, where she is employed in the membership office.
FROM CANCER TO A CURE
Hancock’s long struggle began in May 1997 when she developed hoarseness that would not go away. She was 21, a University of Missouri- St. Louis junior hoping for a career in radio broadcasting, and serious illness was the farthest thing from her mind. Incredibly, cancer was the diagnosis, though she had no family history of the disease and was only a very occasional smoker.
But laryngeal cancer, uncommon in one so young, is not actually rare: Some 13,000 Americans are diagnosed with the disease each year. While smoking is a major risk factor, 5 to 10 percent of patients have never smoked. Why they develop the disease is not yet fully understood, but may have to do with a failure of the immune system to perform routine surveillance and clean-up of stray cancer cells.
In Amy’s case, radiation treatments did not eradicate the cancer, so that December Washington University otolaryngologist Donald G. Sessions, MD, performed surgery to remove her voicebox. He created two separate tracks within her throat: one for eating and another for breathing, the latter connected to a breathing hole or “stoma” in her neck. This laryngectomy was successful—for five and a half years now Amy has been cancer-free—but it also left her without a voice.
“People think of the voicebox as being the voice, but that is only partly true,” says Paniello, associate professor of otolaryngology, who took over Amy’s case after Sessions retired in 2001. “If you put a microphone above your vocal cords, you would just hear the ‘BZZZZZ’ of vibrating tissues. How does that become words? You move your tongue, soft palate, cheeks, lips, even teeth. So if we could reintroduce vibrating tissue, Amy had those other parts intact to convert that vibration into sound.”
Through the years, she tried various ways to reintroduce that needed movement. Following a laryngectomy, some patients learn “esophageal speech”: swallowing a gulp of air and belching it back to create the necessary vibrations. Others use a tiny, implanted device called a tracheo-esophageal puncture (TEP), which diverts air from the windpipe into the throat, again producing the vibrations needed for speech. Neither method worked for Amy, who underwent repeated surgical procedures and Botox injections in an effort to free up tight throat muscles that doctors thought might be hampering the TEP’s effectiveness.
As her five-year anniversary approached in December 2002— the date on which she was considered cured of her disease—Paniello began pondering new ways to help Amy regain more normal-sounding speech. His preferred solution was a larynx transplant, a procedure used successfully in 1998 at the Cleveland Clinic, but Amy’s insurance company rejected the proposal as too experimental.
A PIONEERING PROCEDURE
In spring 2003, Paniello was giving a lecture to otolaryngology residents on ways to rehabilitate laryngectomy patients, when he mentioned a 1990 journal article by a German author on his success with laryngeal reconstruction. Altogether, the surgeon had used it to help 10 patients, mostly at the time of their initial voicebox removal. “As I was speaking,” Paniello says, “I began thinking, ‘Hey this could work for Amy!’”
She was ready as soon as he mentioned it. While her previous surgery had brought some good things into her life—a chance to be keynote speaker at a “Relay for Life” event of the American Cancer Society; the decision to acquire a toy poodle, her darling Macie, as companion and watchdog—it had also led to social constraints.
“I refused to believe that I had to spend my life like that,” Amy says of being speechless.
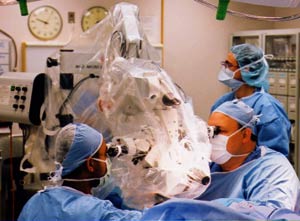
Randal C. Paniello, MD (sitting, right), associate professor of otolaryngology, performs a laryngeal reconstruction on patient Amy Hancock earlier this year. The surgery, the first of its kind done in the United States, gave Amy back the voice she had lost more than five years ago to laryngeal cancer.
This time, her insurance company said “yes.” So at 5 a.m. on May 23, Paniello and his surgical team began the complex reconstruction procedure. Its goal was simple: Just as the TEP does, it would re-create a connection from the airway to the swallowing passage. But instead of using a manufactured device, Paniello would construct the connection, creating a tube of skin that he would implant in her throat.
To find the tissue he needed for it, he would go to her forearm, trimming away a two-inch by two-inch flap of skin, with its blood supply — two veins and one artery—still intact. A graft from her leg would replace the missing arm skin. The prospect of all this did not phase Amy, a veteran of surgical procedures. “I was not at all nervous,” she said afterwards. “I never worried at all.”
Neither did Paniello, who routinely works on the neck and is a specialist in microvascular surgery. After opening Amy’s neck and evaluating her vessels to make sure they would attach well to the skin flap, he and his team moved quickly: shaping, stitching and inserting the tube of skin. A tricky part was creating a trash-can-style “lid” on the tube that would flip up when air needed to pass through, then close so that she could swallow safely, without leaking food into her airway. To achieve the necessary stiffness, he borrowed cartilage from her nose.
There were no unforeseen complications during the surgery, which took less time than the 12 hours that Paniello had predicted: only eight and one-half hours. “Everything fit perfectly,” he says. “It was not a routine procedure exactly, but it went very smoothly—as well as I could possibly have hoped.”
Amy was in the hospital just six days, then at home for
a month-long recuperation that was overseen in part by her mother, who
is a nurse. Amy’s family and many friends gathered at her hospital
bedside to cheer her on during her stay. One wrote
to the Cardinals to request a special treat: a visit from Amy’s
favorite baseball player, second baseman Fernando Viña, who did
drop by to see her. “If there was a moment when I thought I might
die, it was then,” says Amy, who was thrilled.
The real moment of truth was still coming, though. On Monday, June 16—three weeks and three days after her surgery—she was allowed to test her new voice for the first time, before an audience of medical personnel and reporters. First, Paniello removed a plastic tube that he had inserted in her stoma to prevent scar tissue from forming. To talk, she now has to close off the stoma to force air through the new skin tube into her throat. On this morning, he used a catheter to force in the air she needed to speak.
“Oh, my God,” she said tentatively, “thank you.” Soon, amid tears, she was hugging Paniello and speaking in full sentences. The following week she would be fitted with a Provox FreeHands valve that will regulate air flow through the stoma, so that she no longer has to use her thumb to close it off.
“I don’t know if there are words to describe
how I feel,” says Amy, whose speech will always sound gravelly,
though it is much improved over her old mechanical voice. “This
is better than my 16th, 18th and 21st birthdays together. I wanted a voice—and
now I’ve got it.” ![]()
![]()