


 |
 |
 |
|
|
Less is More Innovative treatments offer dramatic benefits compared to traditional surgeries |
||||||
|
Jon Pellechia and his wife, Kellie, have two reasons to celebrate: Earlier this year, Jon was successfully treated for testicular cancer by Robert S. Figenshau, MD, at Barnes-Jewish Hospital. Recently, the couple learned they are expecting their first child. |
Patients diagnosed with a urologic cancer often face the prospect of major surgery — along with a lengthy recovery from a large incision — to cure their disease. Not so at the Alvin J. Siteman Cancer Center at Washington University School of Medicine and Barnes-Jewish Hospital. Whether it's cancer of the prostate, bladder, testes or kidney, most patients can opt for a minimally invasive treatment approach that translates into a shorter hospital stay, less pain and a faster recovery. "Eradicating the cancer is always our first priority," says Gerald L. Andriole, MD, chief of the Division of Urologic Surgery. "But many patients seek out our expertise because they want their cancer treated effectively and they want an easier recovery. In most cases, we can do that for them." In the 1990s, School of Medicine urologic surgeons pioneered the first minimally invasive treatment for urologic cancer: laparoscopic surgery to remove kidney tumors. That advance laid the foundation for today's innovative procedures. "Our urologists really are at the forefront of minimally invasive treatments," says Andriole. "We offer treatments here that are hard to find at many academic medical centers. We're always moving forward."  Managing complexity
Managing complexity
Lymph node removal to assess the spread of testicular cancer is complex, whether done by open or laparoscopic surgery. Robert S. Figenshau, MD, has performed about 40 such laparoscopic procedures in the past five years. None of those patients has experienced a cancer recurrence, which suggests that this technique works as well as traditional surgery, but with the benefit of less pain and faster recovery. 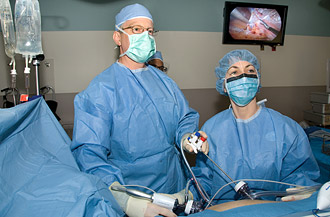 A less invasive approach to lymph node removal Although testicular cancer accounts for just one percent of all cancers in men, it is the most common tumor among those between the ages of 20 and 34. If detected while confined to the testicles, it is almost always curable, says Robert S. Figenshau, MD, professor of surgery. But when it spreads, the metastasis travels a predictable route: first to the lymph nodes near the kidneys, then to the chest and occasionally to the brain. Once the disease metastasizes, the cure rate falls to 80 percent. About half of men with testicular cancer have a type of tumor called a non-seminoma, meaning the cancer originates in cells that eventually become sperm. Even when non-seminomas are detected early, there is still a concern that microscopic tumor cells have spread to the lymph nodes. In such cases, patients often undergo a complex procedure to remove the lymph nodes to confirm the presence or absence of cancer. Typically, the surgery is an open operation with a lengthy incision from the breast bone to the pubic bone. Figenshau, however, is one of the few surgeons in the country with extensive experience performing the procedure laparoscopically via three or four small incisions in the abdomen. "For patients, there's a big gain in recovery," Figenshau says. "They go home the day after the surgery and are back to their normal routine in a few weeks. This compares to a typical three- or four-day stay for the open procedure and several months' recovery time." Whether open or laparoscopic, the procedure is highly complex because surgeons must work around the large blood vessels serving the kidneys, bowel and lower extremities, as well as nerves that control ejaculation. Figenshau has performed about 40 laparoscopic lymph node dissection procedures in the past five years. None of those patients has experienced a cancer recurrence, which suggests that the minimally invasive technique is just as thorough as the open procedure in removing the cancer. Jon Pellechia, 31, of Creve Coeur MO, was diagnosed with testicular cancer in March. He didn't think twice about choosing the laparoscopic procedure over the open surgery. "I did some research," says Pellechia, a physician assistant at Christian Northeast Hospital. "The guys doing the lymph node procedure were at Washington University, and the minimally invasive approach was really a no-brainer for me." Within three weeks, Pellechia was back seeing patients in the hospital ICU where he works. "You don't think of St. Louis as being a big city, but you can get state-of-the-art treatments right here at Barnes-Jewish Hospital."  Targeting tumors
Targeting tumors
Non-surgical options for treating prostate cancer run to two extremes: obliterating the tumor by using the heat of a laser or freezing the prostate to ensure cancer cells are killed. According to Gerald L. Andriole, MD, both procedures effectively destroy the tumor while at the same time minimizing side effects for patients. 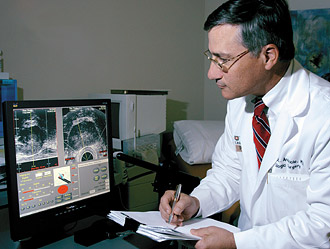 Non-surgical options for tumor destruction While surgery remains the mainstay treatment for prostate cancer, some patients prefer to avoid surgery altogether because of potential complications: namely, urinary incontinence and impotence. For them, Andriole is evaluating focal destruction of only the cancer by two means. Both are in phase III clinical trials: One uses heat to destroy the blood supply of the tumor; the other kills tumors by freezing them. Both have minimal, if any, side effects. In the first procedure, a chlorophyll-based photosensitizing agent is injected into the patient's bloodstream. Once it reaches its target, in this case blood vessels feeding the tumor, the agent is activated by the light of a laser. The activated agent chokes off the blood supply to the tumor, thereby starving the cancer of the nutrients it needs to grow. "Tumors have a unique blood supply, and this procedure is precisely targeted only to blood vessels that feed the tumor, not the vessels that supply the healthy parts of the prostate," Andriole says. The other procedure uses a three-dimensional ultrasound developed in St. Louis to guide the insertion of needles into the prostate that deliver argon gas, essentially freezing the prostate at temperatures lower than -150 degrees F. The prostate is then defrosted and refrozen to ensure that the cancer cells are killed. The entire procedure takes less than two hours. "The technology has greatly improved since cryotherapy was introduced as a cancer treatment," Andriole says. "We can now better target the tumor with only minimal side effects."  Better than by hand
Better than by hand
A computerized system allows surgeons to view a tumor and its surrounding structures in high magnification while maneuvering robotic scalpels, scissors and high-resolution cameras to remove kidney tumors. Surgeon Sam B. Bhayani, MD, pioneered robotic surgery for kidney tumors; he says the procedure is more efficient and precise than either open or laparoscopic surgery for tumors confined to the kidney.  A more "efficient and precise" procedure Instead of standing for hours with his arms raised above the patient, Sam B. Bhayani, MD, sits at a nearby computer console maneuvering joystick-like controls that guide robotic scalpels, scissors and high-resolution cameras to remove kidney tumors. For small cancers, Bhayani excises only the tumor, thereby preserving the function of the healthy portion of the kidney. The procedure appears to be superior to partial nephrectomy performed laparoscopically due to the shorter amount of time blood flow to the kidney must be stopped so the tumor can be excised — about 20 minutes for robotic surgery compared with 30 to 40 minutes for laparoscopic surgery. The longer the blood flow is cut off, the greater the risk that the kidney will not function normally after the surgery. For large tumors that have not spread beyond the organ, Bhayani can remove the entire kidney through one small three-inch incision in the belly button. Other surgeons have used the same procedure to remove kidneys for donation, but never before for cancer. "Robotic surgery is more efficient and precise than either open or laparoscopic surgery for tumors confined to the kidney," says Bhayani, a pioneer in this robotic surgery who has trained surgeons worldwide in the procedure. "Rather than operate with two hands, I can simultaneously control four robotic instruments with mechanical 'wrists' that rotate more than 360 degrees, giving me far greater maneuverability than human hands or laparoscopic instruments." The computer-controlled system also eliminates surgeons' hand tremors, however minute. And the robot provides an exceptional view of the surgical field. The surgeon sees the tumor and surrounding structures in high magnification. Dual miniature cameras restore the depth perception of an "open" surgery, which is lost in standard laparoscopy. Patients who have had the robotic procedure have quicker recoveries than with open surgery — one day in the hospital versus five. Because surgeons remove the entire tumor using robotic surgery, there's no need for further chemotherapy or radiation treatments, Bhayani says.
A better way to treat bladder cancer

Like other minimally invasive approaches, the robotic procedure for the treatment of bladder cancer seems to work as well or better than open surgery, with the added benefit of faster recovery time for patients. Adam S. Kibel, MD, is one of the few surgeons in the nation currently offering the robotic option. At Barnes-Jewish Hospital, about half of all bladder cancer surgeries are now performed robotically; that number is expected to grow substantially over the next several years. 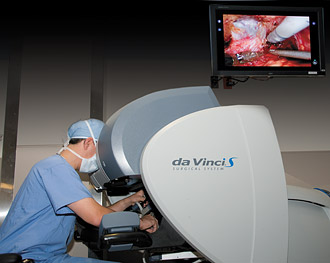 Taking robotics to other bodily organs Robotic surgery also has entered the realm of treatment options for bladder cancer. More than one year ago, Adam S. Kibel, MD, professor of surgery, began using robotics for patients who have cancer that has invaded the deep layers of the bladder wall. In addition to the bladder, the surrounding lymph nodes are removed as well as the prostate and seminal vesicles in men and the uterus, ovaries and part of the vagina in women. In women, the organs can be removed via the vagina. "It's definitely major surgery," says Kibel. "Our early results suggest that the robotic surgery is as good as open surgery for curing the cancer, with the advantage that patients recover substantially faster with less pain compared to the open surgery." Only a limited number of U.S. surgeons currently perform the procedure robotically. The benefits are substantial: less blood loss, less pain, a shorter hospital stay and fewer post-surgical complications. About half of all bladder cancer surgeries at Barnes-Jewish Hospital are now performed robotically, and that number is expected to grow substantially in the next several years. Because bladder cancer is more common among patients who generally have slower recoveries — those over age 60 and current or former smokers — the shorter recovery time for robotic surgery can be a big consideration when patients contemplate the operation. |
|||||