
-

- Hip preservation
- cRAWdads
- The Power of Two
- Mapping the brain
- Fulfilling a dream
- Siteman’s NCI designation renewed
- Student Profile: Tassy Hayden
- Save your breaths
- Children's Sustainability Art Contest
- Cardiovascular disability benefits
- Bee safe
- Distinguished professorships
- A Passion for Education
- Coffee & Sound


A medical mystery began one summer’s day on a Missouri waterway when someone ate something that most Americans would never think of putting in their mouths — that is, not unless it had first been sauteed, baked, boiled or fried.
Before this illness was diagnosed at Washington University School of Medicine, only seven such cases had ever been reported in North America, where a parasite, Paragonimus kellicotti, is common in crayfish.
Cooking destroys the parasite. But when mammals consume raw crayfish, the illness paragonimiasis is the result. It can cause fever, cough, chest pain, shortness of breath and extreme fatigue. Diagnostic clues also include elevated levels of a particular type of white blood cell and fluid around the lungs and sometimes the heart.
The infection is generally not fatal and is easily treated, if it is recognized. The story of this unusual case highlights the importance of getting a thorough medical history in order to arrive at an accurate diagnosis.
“We’re all taught this in medical school,” says infectious diseases specialist Thomas C. Bailey, MD, professor of medicine, “but increasingly physicians can rely too heavily on technology to make a diagnosis without listening to what patients — or patient’s family members — are telling them.”
There also can be value in the redundancy of a medical school/teaching hospital approach, he says, where multiple people take a patient’s history.
“Important details may be uncovered by one person but not another,” Bailey says. “And it’s not uncommon for a medical student — particularly the smart students here — to uncover a critical clue.”
CONTINUED BELOW
Division of Infectious Diseases
Centers for Disease Control and Prevention Morbidity and Mortality Weekly Report
Missouri Department of Health and Senior Services

More than 30 species of crayfish live in the rivers, streams, lakes and ponds of Missouri. Some of them, such as the spothanded crayfish (Orconectes punctimanus), left, can harbor a troublesome parasite. Paragonimus kellicotti begins its life in a snail and then infects crayfish, but only causes a dangerous infection if it is ingested by mammals — including dogs, cats and humans — who eat the crayfish raw.
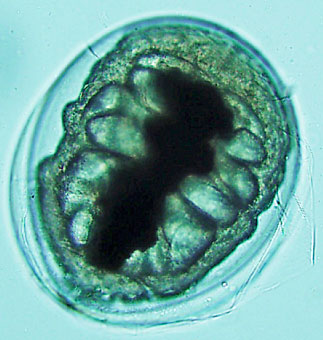
Once inside the human intestine, the infectious-stage larva, called metacercaria, right, leave their protective cysts and migrate to the lungs, where it takes about six weeks for them to develop into sexually mature adult worms, or flukes. The larva can also migrate to the brain, causing severe headaches or vision problems, or under the skin, appearing as small, moving nodules.
Infectious disease doctors at the School of Medicine routinely play the role of medical detectives, tracking down clues to diagnose unusual illnesses in patients. But of all the obscure diseases they see, this one stood out as truly bizarre.
It began when a 31-year-old man walked into Barnes-Jewish Hospital’s emergency room with fever, chills, shortness of breath and a cough. He already had been evaluated at a local urgent care center; doctors sent him home after tests for mononucleosis and strep throat came back negative.
Several days later, when his symptoms had not subsided, the patient went to an emergency room near his home for treatment. Results of blood tests, a chest X-ray and a lumbar puncture revealed nothing out of the ordinary. Because he had been on a camping trip several weeks earlier, doctors prescribed a seven-day course of an antibiotic to treat a suspected tick-related infection.
But a week later, the patient’s symptoms had worsened. He also was experiencing chills, rigors, drenching night sweats and headaches. This time, doctors prescribed another antibiotic, to no avail. Along with the shortness of breath, he had developed chest pains and was losing weight.
By the time the patient arrived at Barnes-Jewish Hospital, he’d had symptoms for more than two weeks. In the emergency room, doctors learned that he had visited Mexico six weeks before his symptoms — which mirrored those of malaria — developed. They also were worried about the possibility of a blood clot in the lung.
Doctors performed blood tests, a chest X-ray and a CT scan. As a precaution, the patient was prescribed an anti-malarial medication and admitted to the hospital for a consult with an infectious diseases physician. The chest X-ray and CT scan showed fluid around the lungs and a mass in the right lung. Blood tests revealed elevated levels of eosinophils, a type of disease-fighting white blood cell. The findings suggested that the patient might have cancer, possibly lymphoma, which is associated with lingering fever and a high eosinophil count. But they could also point to an autoimmune disease, allergy or even a parasitic infection.

GOOD EATIN’
For birds, that is, who unlike mammals are immune to the parasitic infection.
“You have to be a bit of a detective and remain open to all the clues,” says Bailey, who later diagnosed and treated the patient. “As doctors, we are taught that unusual presentations of common illnesses are far more common than classic presentations of rare diseases. In this patient’s case, the duration of his symptoms already defined him as having something unusual, if not rare.”
A fourth-year medical student was the first to see the patient after his admission to the hospital. She took a careful history and then examined him.

Infectious diseases specialists Michael A. Lane, MD, left, and Gary J. Weil, MD, examine a crayfish in the laboratory.
The patient could not recall anything remarkable about his trip to Mexico or a recent camping trip on the Current River that might explain his illness. As an aside, his wife, who was in the room, casually mentioned that he had eaten two raw crayfish — on a dare — during the camping trip.
The student noted the information and discussed the case with Bailey a short time later. Together, they went over the physical exam, laboratory results and the patient’s medical history. Then, she told Bailey about the raw crayfish.
“That was a major clue,” says Bailey, who recalled that in Asia eating raw or undercooked crabs can cause a parasitic infection. He quickly Googled crayfish, along with some of the patient’s symptoms, and up popped reports of a rare parasitic lungworm infection called North American paragonimiasis, which had been described in patients who had eaten raw crayfish. The scenario fit perfectly. “I said, that’s it,” Bailey recalls. “That’s what he’s got.”
Bailey prescribed the appropriate medication, even as he and other doctors worked to rule out other, more common illnesses. However, the patient’s symptoms began to improve within two days and completely resolved within two weeks.
But the paragonimiasis story doesn’t end with this patient’s case. Infectious diseases doctors at the School of Medicine have been diagnosing an increasing number of cases of the illness in recent years in patients who have consumed raw crayfish caught in Missouri’s rivers and streams. Five such cases have occurred in the past year alone.
Thomas C. Bailey, MD, recounts a classic case showing the value of an in-depth patient history.
“The infection is very rare, so it’s extremely unusual to see this many cases in one medical center in a relatively short period of time,” says infectious diseases specialist Gary J. Weil, MD, professor of medicine and of molecular biology, who treated some of the infected patients.
Because community doctors are generally not aware of paragonimiasis, many of the patients seen at the medical center had received multiple treatments for pneumonia, courses of steroids for possible autoimmune diseases, or had undergone invasive procedures before they were referred to Barnes-Jewish or St. Louis Children’s hospitals for treatment. One even had his gallbladder removed.
The rising rate of paragonimiasis infections prompted the Missouri Department of Health and Senior Services to issue a health advisory about the infection to alert doctors across the state. The department also printed posters warning people not to eat raw crayfish and placed them at campgrounds and canoe rental businesses.
The message for physicians is to consider paragonimiasis in patients who present with chronic cough, fever, fatigue and elevated eosinophils.
“Some of the invasive procedures could have been avoided if the patients had received a prompt diagnosis,” says infectious diseases specialist Michael A. Lane, MD, instructor of medicine, who also treated some of the infected patients. “We hope more doctors will now have this infection on their radar screens.”
It’s unclear why more cases of paragonimiasis are being diagnosed, but doctors and researchers at Washington University continue to study the parasite and have made progress in developing better diagnostic tests for the infection.
Diagnosing such interesting cases is what makes being an infectious diseases doctor so interesting, says Bailey.
“Every time you see a new patient,” he says, “you have to be open to the possibility that the diagnosis could be something highly unusual.”
Nature images courtesy of Missouri Department of Conservation.




