-

- Hip preservation
- cRAWdads
- The Power of Two
- Mapping the brain
- Fulfilling a dream
- Siteman’s NCI designation renewed
- Student Profile: Tassy Hayden
- Save your breaths
- Children's Sustainability Art Contest
- Cardiovascular disability benefits
- Bee safe
- Distinguished professorships
- A Passion for Education
- Coffee & Sound

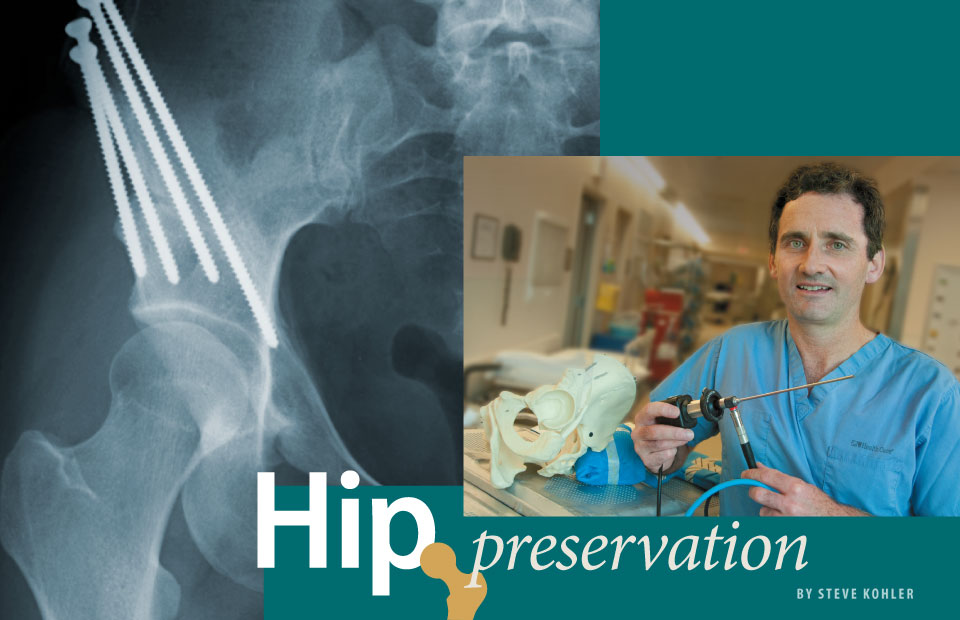
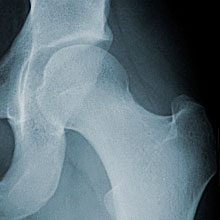
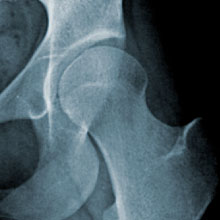
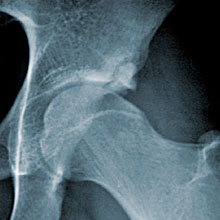
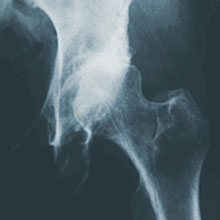
Hip disorders can be treated long before total replacements are needed. John C. Clohisy, MD, specializes in these radical surgeries, such as the one at left that corrected an unstable hip joint.
Department of Orthopaedic Surgery
Center for Adolescent and Young Adult Hip Disorders
Repairs beat replacing
Click images below to learn more
Hip surgery isn't just for the elderly anymore. And for good reason.
Robert O’Dell was a 23-year-old U.S. Marine and a competitive martial artist in the winter of 2007, when pain in his hips began to intensify and interfere with his mobility. With a family history to alert him and a diagnosis of bilateral, developmental hip dysplasia — shallow hip sockets — he feared that degenerative arthritis in his hips was around the corner, followed eventually by two total hip replacements. He had a vision of himself “in a wheelchair at 30,” he says.
And had it been just 10 years earlier, O’Dell might have been correct. Historically, hip disease in young people was treated non-surgically as a pain issue, anticipating the progression of osteoarthritis, culminating in hip replacement. But recently, thinking about young people and hip pain has undergone a sea change. “We didn’t fully understand or know how to diagnose and treat young patients. But over the past decade we’ve developed an understanding of osteoarthritis of the hip and what leads to it. Now we know more about the anatomy of the hip and the effects of mild deformities” says John C. Clohisy, MD, the Daniel C. and Betty B. Viehmann Distinguished Professor of Orthopaedic Surgery and director of the Center for Adolescent and Young Adult Hip Disorders.
Instead of waiting until advancing arthritis dictated hip replacements, Clohisy, who is on the medical staffs of Barnes-Jewish and St. Louis Children’s hospitals, performed a periacetabular osteotomy on O’Dell’s left hip in July 2009, and on the right side in January 2010.
CONTINUED BELOW
In the procedure, Clohisy makes a series of bone cuts to loosen the hip socket from the pelvis. The hip socket is then repositioned to create a deeper, more stable, hip joint.
Because his condition was corrected before the joint deteriorated, O’Dell says he had 100 percent correction on both sides. “Miracle surgery,” he calls it. He can run and has earned a score of 297 out of a possible 300 on the U.S. Army’s physical fitness evaluation. He left the Marines and is in the process of being hired by Homeland Security as a border patrol agent, a position in which he can use his experience and restored physical abilities in service to the country.
As it was in O’Dell’s case, the most common cause of dysplasia is a developmental deformity. And although O’Dell’s high level of activity and athleticism may have called early attention to the problem, they were not causal, Clohisy says.
Impingement, another form of hip disease frequently treated at the center, is also most often traceable to a developmental deformity of the hip. It occurs when the socket is too deep or the ball is misshapen. When the hip flexes, abnormally high friction causes pain and eventually damages the ball and/or socket surfaces or the soft tissue around the rim of the socket. Common in athletes, the problem is frequently misdiagnosed — sometimes even as a groin injury. Of course, the rest and pain management prescribed for a pulled muscle do not effectively treat hip impingement.

Martial arts training pushes Robert O’Dell’s hip joints to the extreme. His shallow hip sockets were rebuilt to make deep squats such as these pain-free.
However, effective surgical treatments have been developed, and diagnosis is now much more precise. At the center, the most common treatment is hip arthroscopy, a procedure in which a fiber-optic camera is inserted through a small incision, allowing the surgeon to visualize the hip. Specialized instruments facilitate repair and some recontouring of the natural bones. In more complex cases, open surgery may be called for, to correct major deformities that are not accessible with arthroscopic techniques. Both arthroscopic and open surgical techniques can be very effective in relieving the impingement and improving hip function.
The purpose of these rapidly advancing approaches and techniques is universally to relieve pain, improve function and delay or perhaps even prevent the onset of arthritis, according to Clohisy. Taken collectively, they go by the name “hip preservation surgery.”
But that goal is not always possible. Rachel Van Winkle was only 9 years old when she was diagnosed with systemic juvenile rheumatoid arthritis, a chronic autoimmune disease that causes inflammation of the joints and their protective tissues. A progressive illness, it leads to destruction of the joint.
Van Winkle was 14 when she had gotten as much use as possible out of her hips, and pain told her and her physicians that something had to be done. At the center, the physicians found her arthritis was advanced and the natural hip joints were ruined. They determined that complete hip replacements were called for — the right hip at age 14 and the left three years later.
"The purpose of these rapidly advancing approaches and techniques is universally to relieve pain, improve function and delay or perhaps even prevent the onset of arthritis."
—John C. Clohisy, MD
Van Winkle’s hip replacements are five years in her past, and she is preparing to graduate from college. She now sees Clohisy on a two-year schedule, and together they expect that she will get 20, or even more, years of use out of the joints.
Any decision to replace a young person’s hip joint comes only after careful consideration by the center’s members. According to Heidi Prather, DO, associate professor of orthopaedic surgery and chief of the section in physical medicine and rehabilitation, when Clohisy created the center and invited participation of multiple disciplines, it was not just lip service. “The group is unique; it fully integrates those who are not surgeons. We work together to evaluate, treat and research, looking at each problem from every angle.”
Prather sees all patients, even those referred directly to one of the surgeons and those with undiagnosed hip pain. “There’s a lot of back and forth. In the clinic we share, I often convince surgeons to try something diagnostically,” she says. “We take great care to be specific about the patient’s history and physical exam. We need to be sure that what we see on an image is really the problem; that we are imaging the right thing.” Members’ close cooperation and open communication contributes to the center’s clinical success, she says.

Some young hips do require full replacement. The recipient of two artificial hips after her diagnosis for systemic juvenile rheumatoid arthritis, Rachel Van Winkle can expect another few decades’ use before new hips will be needed.
A third principal, Perry L. Schoenecker, MD, professor of orthopaedic surgery and chief of pediatric orthopaedics at St. Louis Shriners Hospital for Children, performed joint preservation surgery on adults for 30 years and now concentrates on children, rounding out the comprehensiveness of the center and bringing care to that previously underserved population.
He says the collaboration in the group goes well beyond what is common in most such centers. He and Clohisy often work together in the operating suite as co-surgeons and have performed more than 300 periacetabular osteotomies. “It’s synergistic,” he says. “When things get difficult, the combination sees us through. We’re both technically demanding of our craft, and where a lone surgeon might settle for a less-than-perfect solution, one of us often says, ‘I think we can make that better.’”
To push back the number of young patients who need replacements and advance hip preservation treatments, members participate in a range of research projects. A multidisciplinary group studies diagnosis, treatment and outcomes, involving physical therapists, biostatisticians, physiatrists, radiologists and basic scientists looking at the progression of pre-arthritic hip disease.
Center member Linda J. Sandell, PhD, the Mildred B. Simon Research Professor of Orthopaedic Surgery and professor of cell biology and physiology, is an expert in osteoarthritis, studying the mechanisms that mediate joint deterioration. Her clues: tissues removed from affected joints and their proteins and enzymes that lie outside the norm.
Members also lead the eight-center Academic Network of Conservational Hip Outcomes Research (ANCHOR) study group which enrolls more than 500 patients each year in various studies. Clohisy and his multicenter colleagues staff the coordinating center located at Washington University.
“What we’re learning is that there are major advantages to preserving the joint,” he says. “Hip replacement may have to be done, but we don’t want to do it in the patient’s teens, 20s or 30s unless there is no other choice.”