
Co-inventor of promising nanofiber: Matthew R. MacEwan

Co-inventor of promising nanofiber: Matthew R. MacEwan
Matthew R. MacEwan is no ordinary medical student. The neurosurgeon-to-be, a student at the School of Medicine, also is pursuing a doctorate in biomedical engineering at Washington University. And, at 29, he recently started his own local company, Retectix LLC, aimed at revolutionizing the surgical mesh used in operating rooms worldwide.
The company’s lead product, invented by MacEwan and Jingwei Xie, PhD, a former postdoctoral researcher in engineering, is a synthetic polymer mesh made of synthetic nanofibers. The mesh was developed to repair defects in the membrane surrounding the brain and spinal cord, but also could be used to mend tissues as well. The nanofiber material has the potential to make operations easier for surgeons and reduce the rate of complications experienced by patients
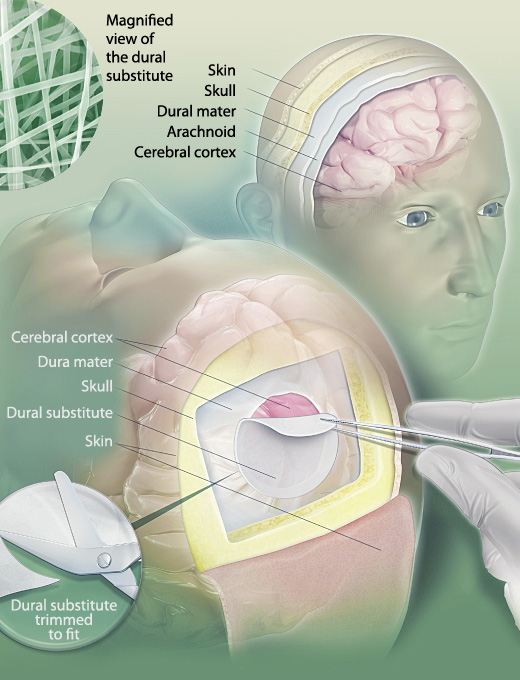
Existing surgical mesh used to repair the protective membrane that covers the brain and spinal cord is thick and stiff, making it difficult to work with. But the novel material MacEwan and Xie developed is thin and flexible and more easily integrated into the body’s own tissues.
“It’s almost like a cloth,” MacEwan says. “But it’s designed on a nanoscopic scale. To put that into perspective, every thread of the mesh is hundreds to thousands of times smaller than the diameter of a single human cell.”
The technology’s promise has caught the attention of the business world. In 2011, MacEwan won the Olin Cup, sponsored by Washington University’s Skandalaris Center for Entrepreneurial Studies. In June he won the Licensing Executives Society Foundation’s International Graduate Student competition in London, and last November, the Idea to Product Global Competition in Stockholm. The winnings of more than $100,000, along with other investments and in-kind services, have helped MacEwan get the company off the ground.
The nanofiber material developed by MacEwan and Xie, now a senior scientist at Marshall University in West Virginia, along with collaborators Younan Xia, PhD, the James M. McKelvey Professor of Biomedical Engineering, and Zack Ray, MD, now an attending neurosurgeon at the School of Medicine. MacEwan has worked closely with Washington University’s Office of Technology Management, which has filed patents on the technology.
“We’ve taken the whole idea of surgical mesh and pushed it into a new direction,” MacEwan says. “It’s not just a foreign material you’re putting into the body. The nanofabricated nature of the mesh creates a scaffold that cells can easily penetrate and populate to recapitulate the body’s tissues.”
The surgical mesh looks like gauze but feels sticky, like a spider web. It is typically composed of multiple layers of nanofibers and can be cut to size for different uses. Once the mesh is placed in the body, cells grow along the individual nanofibers, which gradually degrade in nine to 12 months, leaving only the body’s own tissue in their place.
One advantage of the new technology is that different patterns of nanofibers can be created in the mesh to promote the healing of different kinds of wounds. For example, in a starburst pattern used to repair ulcers and other circular wounds, the nanofibers originate from a central point and radiate outward. This encourages cells to migrate and grow toward the center of the wound. For linear defects like tears and incisions, nanofibers can be aligned perpendicular to the wound, encouraging cell growth across the injury, which provides reinforcement to the new tissues.
MacEwan is currently evaluating the product in animal models, a first step toward gaining U.S. Food and Drug Administration approval. Preliminary studies indicate the nanofiber material is safe and effective; MacEwan is hopeful that clinical trials in patients will begin later this year.
For now, MacEwan is finishing his doctorate and has two years left before he receives his medical degree. He’s planning a career in academic medicine, where he can spend time in the laboratory and the operating room. There, he hopes to use the nanofiber surgical meshes he developed to improve the care and surgical outcomes of his own patients.
“At Washington University, I have continually focused on moving discoveries beyond the laboratory,” MacEwan says. “I hope to see this technology have a positive impact on many patients. Nothing would be more thrilling.”