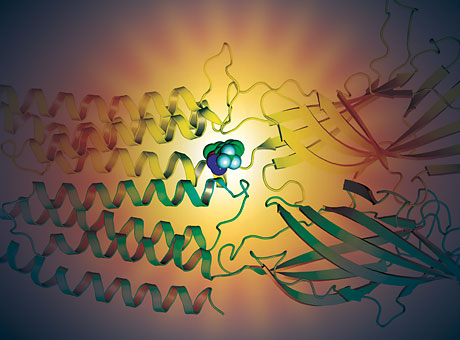
Researchers used a photoanalogue of propofol to identify where it binds to GABAA receptors. The small circles show the site.

Researchers used a photoanalogue of propofol to identify where it binds to GABAA receptors. The small circles show the site.
Researchers at Washington University School of Medicine and Imperial College London have identified the site where the widely used anesthetic drug propofol binds to receptors in the brain to sedate patients during surgery.
Until now, it hadn’t been clear how propofol connects with brain cells to induce anesthesia. The researchers believe the findings, reported online in the journal Nature Chemical Biology, eventually will lead to more effective anesthetics with fewer side effects.
“For many years, the mechanisms by which anesthetics act have remained elusive,” explained co-principal investigator Alex S. Evers, MD, the Henry E. Mallinckrodt Professor and head of the Department of Anesthesiology. “We knew that intravenous anesthetics, like propofol, act on an important receptor on brain cells called the GABAA receptor, but we didn’t really know exactly where they bound to that receptor.”
Short-acting propofol often is used in surgical patients. It wears off quickly and is less likely to cause nausea than many anesthetics. But the drug isn’t risk-free. Potentially dangerous side effects include lowered blood pressure and interference with breathing.
To understand how propofol induces anesthesia during surgery, scientists have tried to identify its binding site within the gamma-aminobutyric acid type A (GABAA) receptor on brain cells. Activating these receptors — with propofol, for example — depresses a cell’s activity.
Evers’ laboratory teamed up with a group at Imperial College led by Nicholas P. Franks, PhD, professor of biophysics and anaesthetics. The group had created a photoanalogue of propofol that behaves in precisely the same way as propofol and contains a labeling group that permanently attaches to its binding site on the GABAA receptor when exposed to a specific wavelength of light.
In creating the analogue, it’s as if the researchers put a tiny hook onto the molecule so that when it binds to the GABAA receptor, it grabs onto the receptor and won’t let go.
“The next step was to extract the receptor, cut it into pieces and identify the precise piece of the protein where the propofol analogue had attached to the receptor. This was the tricky step that the Evers group at Washington University had perfected,” Franks said.
Evers and Franks believe this technique has implications for other types of drugs beyond anesthetics, such as psychiatric agents and anti-seizure drugs.
“By understanding precisely what the binding sites look like on the proteins that induce those potential problems, we eventually hope to design and select for drugs that have the benefits we want without dangerous side effects,” Evers said.