
One to grow on: Dillon, who was treated for congenital pulmonary airway malformation, with his mom, Carol Waeckerle, and Fetal Care Center co-directors Barbara B. Warner, MD, MSCE, left, and Lisa M. Bernhard, MD.
Photo by Robert Boston

When ultrasound screenings in pregnancy indicate that babies’ tiny systems may be developing irregularly, or family medical histories suggest anomalies may occur, doctors from around the region refer mothers to the Fetal Care Center (FCC). With their hopes badly shaken for an uneventful pregnancy and a healthy baby, families arrive at the center longing for answers, for interventions from medical science, for hope. And they find these things, in their many forms, as they are guided through a compassionate sequence of physical and emotional care.
FCC medical co-director and neonatologist Barbara B. Warner, MD, MSCE, specialized in newborn medicine because she was drawn to working with ill and premature newborns and their families. “Helping and supporting is a great privilege,” says Warner, professor of pediatrics in the Department of Pediatrics, whose neonatal group is ranked among the top three in the United States, according to U.S. News & World Report.
Adds medical co-director and medical geneticist Lisa M. Bernhard, MD, “With our comprehensive, in-depth care, we give babies their very best possible chance. We do all we can to make these terribly stressful months in families’ lives as easy and as seamless as possible.”
Fetal Care CenterThe Fetal Heart CenterSt. Louis Children’s HospitalNewborn Intensive Care Unit (NICU)

Focused on patients and the family
Although every major medical center has some type of coordinated fetal care, center founder and director George A. Macones, MD, MSCE, explains the goal of the Fetal Care Center, which is a joint effort of Washington University School of Medicine, Barnes-Jewish Hospital and St. Louis Children’s Hospital.
“We are fully focused on our patients — mother and baby — and the family. We bring very upset parents into the Fetal Care Center, which is part of a complex quaternary medical center made up of world-class physicians and hospitals, but we make sure they get lots of information and know we’re taking complete care of them through this difficult time,” says Macones, the Mitchell and Elaine Yanow Professor, head of the Department of Obstetrics and Gynecology, and that department’s director of maternal–fetal medicine and ultrasound. “That special care isn’t just during the initial evaluation: It extends through pregnancy, delivery and afterward.” Macones is internationally known as a clinician and perinatal clinical researcher.
Personalized attention
Overseeing all the personal attention patients receive is a nurse coordinator at the FCC or, if a cardiac problem is involved, from the Fetal Heart Center, part of the St. Louis Children’s and Washington University Heart Center. Nurse coordinators like Christine Hoover, BSN, RN, are a resource and partner throughout the journey to delivery. “We’re with families from the time they arrive until we walk them to their car,” she says. Nurse coordinators accompany mothers to all tests, meetings and consultations, “making sure everyone is on the same page and answering families’ questions.
“We also tour the facilities to help parents feel comfortable,” Hoover continues. “If we see it’s too much, we stop.” Recently a mother told Hoover, “Yes, I really want to see the NICU.” But when they entered the hushed, darkened room, where sick infants slept next to sophisticated instrumentation and some parents sat crying, she burst into tears.
“We postponed the rest,” Hoover says. “We always act on the patient’s wishes, including rescheduling appointments and obtaining temporary physician privileges at Barnes-Jewish if a patient wants her own obstetrician to deliver her baby. As many as 12 extended family members have attended consultations! We do everything we possibly can to make things better.”
Comprehensive assessment
Diagnosing a fetal anomaly that confirms or modifies a referring physician’s finding — or discovering that the fetus is normal — is the work of the ultrasound and genetics side of maternal–fetal medicine. “When we find an abnormality, we look very carefully for other problems, because very often when one exists, other conditions are present that may not have been identified,” says Bernhard, assistant professor of obstetrics in the Department of Obstetrics and Gynecology’s Division of Maternal–Fetal Medicine (MFM). “Then we discuss what, with patient consent, should be done — such as amniocentesis or a fetal MRI — to try to discover why a particular birth defect has occurred.” Following the comprehensive assessment, “We go in right away to talk with the parents, and then we contact the referring physician.”
Jacqueline Turner, MD, of West End Ob/Gyn, in St. Louis, sends all her pregnant patients to the ultrasound and genetics group for their early, routine ultrasound. “We prefer that those physicians do the screening,” she says, “because if there’s an issue, we know they’ll find it. If something major is wrong, they actually call me at the time they’re doing the ultrasound.” For families and referring doctors alike, she adds, the FCC is a “great service.”
Personal touch: Nurse coordinator Christine Hoover, left, walks mom Theresa Clark through her scheduled visits in the Center for Advanced Medicine.
Photo by Robert Boston
Evidence-based, safe care
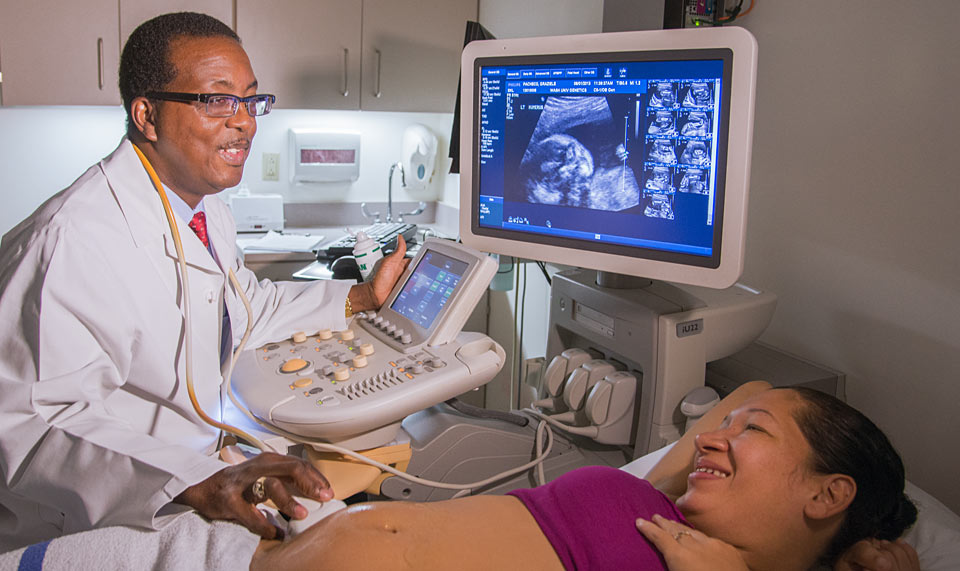
Leading the ultrasound and genetics team is maternal–fetal medicine specialist Anthony A. Odibo, MD, MSCE, whose ultrasound and fetal-abnormality research is known worldwide. Odibo is also skilled in treating Twin-Twin Transfusion Syndrome (TTTS), which can affect identical twins who share a single placenta. In this condition, one twin transfuses blood to the other, producing anemia and drastically slowed growth in the donor and excessive growth and blood volume in the recipient.
He and his colleagues also use endoscopic surgery to place shunts in tiny obstructed bladders, and they correct amniotic band syndrome, wherein a strand of the amniotic sac membrane has wrapped itself so tightly around the baby that loss of digits or blocked placental blood delivery can occur.
“We provide evidence-based, safe care,” says Odibo, professor of obstetrics and gynecology and vice chair for women and fetal imaging. “Before we use new procedures in which some risk may be involved, the situation must be one in which we know definite evidence exists that prenatal surgery or intervention is better than doing nothing. That’s where we differ from some of our competitors.”
Anthony A. Odibo, MD, MSCE, professor of obstetrics and gynecology, leads the Fetal Care Center’s ultrasound and genetics group. Ultrasound is one of a range of diagnostic tools used to screen pregnant patients like Graziele Pacheco.
Photo by Robert Boston
Specialized in fetal care and pediatrics
Fetal cardiac problems account for about 50 percent of anomalies seen at the Fetal Care Center. In all cases, once the MFM specialists have examined the heart and the whole baby, fetal cardiac nurse coordinator Kym Galbraith, BSN, RN, accompanies mother and family to the adjacent Fetal Heart Center. There, pediatric cardiologists use echocardiography in a 30- to 60-minute noninvasive test to check cardiac function and structure.
“Our heart center is completely full-service,” says Caroline K. Lee, MD, assistant professor of pediatrics, associate director of the Pediatric Cardiology Fellowship Program and director of fetal cardiology. “Every heart specialty is represented.”
The professional roster at Children’s, a leading transplant center, includes three electrophysiologists, not found at many centers, three cardiac catheterization physicians and 50 specialists who can administer extracorporeal membrane oxygenation (ECMO), an advanced treatment that does the work of heart and lungs. The hospital’s pediatric subspecialists represent every existing category, ready to step in as needed before and after delivery, and newborn neurology provides neurological imaging, monitoring and consultation.
When a sick infant is born at Barnes-Jewish Hospital, with every necessary expert in attendance, the child is stabilized and placed in a life-supporting isolette. A specialist takes the newborn and father to the Newborn Intensive Care Unit (NICU), where a neonatology nurse coordinator waits.
The mother and an attendant visit shortly afterward. Seeing their infant for the first time marks the start of a second, hopeful journey for many parents, who have already learned about planned treatments or surgeries.
But about 20 percent of FCC families, says Warner, “have infants with lethal disorders. And while we may not be able to reverse that process, we provide the baby with warmth, pain medication — whatever he or she needs to be comfortable. And if a baby will die, we can still provide the family with a meaningful experience with their child that they’ll always cherish.”
Honoring families‘ wishes
Regardless of the prognosis, Joan L. Rosenbaum, MD, director of palliative care and professor of pediatrics, is central to providing comfort and support. Rosenbaum gets to know the families personally in the months before birth and helps them identify their wishes. Among these may be spiritual requests, such as wanting their infant baptized.
“Joanie writes a beautiful letter detailing the parents’ wishes, so that they are communicated to everyone involved in their infant’s care,” says Hoover, the nurse coordinator. “Just last week, a family from southern Missouri met with her. The first hospital they visited wouldn’t allow them to have a photographer and other simple things that would mean everything to them. They decided to come here for care because they felt, in the mom’s words, that we honored her and her baby and valued them both.”
As the FCC looks to the future, one goal is overarching. And that, as Lisa Bernhard puts it, is further refining and focusing on the patient experience.
“Our physicians and staff care so much more than our patient families even realize,” says Christine Hoover.
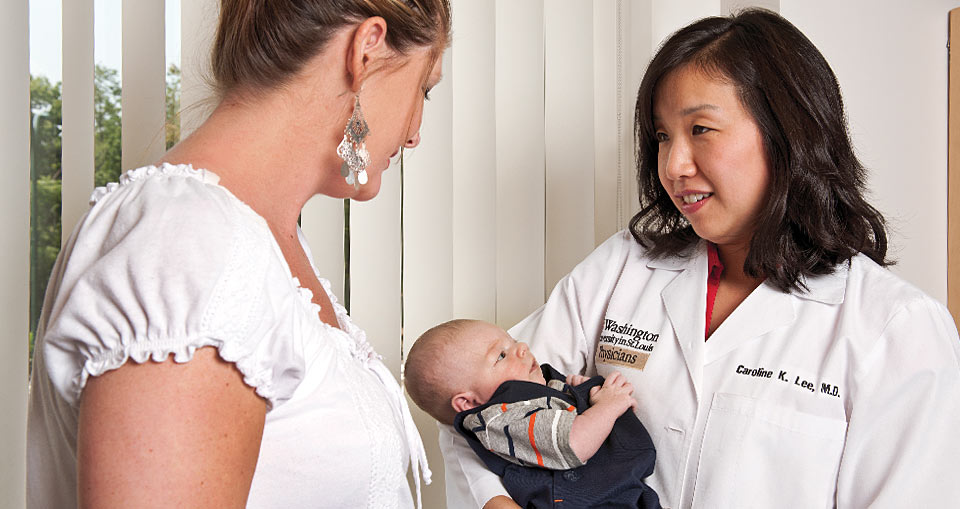
Caroline K. Lee, MD, consults with mother Misty Nutter and baby Austin Rakers.
Courtesy of St. Louis Children's Hospital
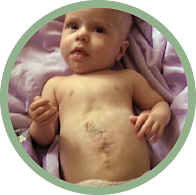
Go, Team Hayden!
Hayden Hoskins is just one of the many infants cared for at the Fetal Care Center. Ultrasound revealed Hayden’s omphalocele; his organs were growing outside his belly. Parents Andy and Kelsea were referred to the FCC. After Hayden was delivered at Barnes-Jewish Hospital, he was rushed to the NICU at St. Louis Children’s Hospital. Five months later, a surgical team placed his organs internally. Today, Hayden has a lot to smile about.


The promise of a healthy pregnancy sometimes changes in a heartbeat. The Fetal Care Center (FCC) helps these mothers and families walk their more challenging paths, offering world-class medicine in a sensitive, caring environment.
Cause for concern
A routine checkup near the end of the first trimester indicates a possible anomaly in the pregnancy. The woman’s physician refers her to the FCC for further evaluation.
All things considered
A nurse coordinator welcomes the family and escorts them through the diagnostic sessions. Single problems can signal multiple issues; tests range from imaging to genetics and more.
Family matters
The FCC responds with sensitivity and respect to families’ needs during these difficult, stressful days. The prognosis is carefully considered and support provided for making choices and moving forward.
The journey continues
In utero interventions may be essential for further diagnoses or to stabilize the pregnancy. The care team coordinates an evidence-based medical plan that maximizes health benefits and minimizes risks.
The big day arrives
A team of specialists stands ready to deliver skilled care before, during and after delivery. Every baby has a spectrum of special needs; the team works to meet those needs and honor the family’s wishes.
Newborn and beyond
Very sick infants receive optimal care during their too-short lives. Many more babies will benefit from specialty procedures during the months ahead, helping ensure lifetimes of happy birthdays.






