
LEARN MORE

Scripted scenarios, intelligent improv and informed feedback hone the clinical skills of tomorrow’s physicians
BY DEB PARKER
ED REGGI HAPPILY REPORTS THAT, since 2009, he has suffered from tuberculosis, bouts of depression, stomach ulcers, acid reflux, diabetes, sleep apnea, migraines, night sweats, chest pains and high blood pressure. He looks forward to developing many more ailments in the coming years.
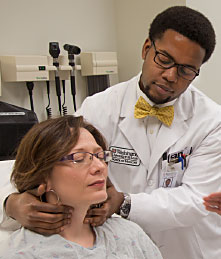
Committed to helping medical students become better doctors, he is one of nearly 70 local professional actors working as standardized patients (SPs) at Washington University School of Medicine. They portray real patients, and repeatedly subject themselves to physical exam by inexperienced hands. In this safe practice environment, medical students hone their clinical skills.
Through this immersive program that builds in complexity over four years, students undergo a stunning transformation. Here, they learn to get comfortable touching and examining patients, taking histories, asking personal questions and writing notes. By the program’s conclusion, the students will have practiced delivering a terminal diagnosis.

Physician, know thyself
As the process unfolds, students learn more about who they are as individuals and how they can better connect with their future patients. In a benefit not afforded in the real world, SPs are trained to critique the students’ techniques — breaking character after a simulation and telling them exactly what it felt like to be their patient.
Program organizers say, in the real world, most people “vote with their feet”: If displeased with a doctor’s lack of attentiveness or communication, they simply won’t come back or won’t follow health recommendations.
“Patients today tell us, ‘I want you to be a good diagnostician and practice evidence-based medicine, but that’s not sufficient. I also want you to be able to talk to me,’” said Dehra A. Glueck, MD, assistant professor of psychiatry and medical director of the Standardized Patient Program. Glueck also served on a communications skills task force for the National Board of Medical Examiners.
The initial, one-on-one standardized patient encounter happens early in the first year. The student must suspend disbelief, read the door note, knock and enter. A standardized patient, already in character, awaits.
The challenge: ask the right questions, keep the patient on topic, gather information, respond to concerns and be empathic.
“This is about being fully present in the moment,” said Jamie Pitt, Standardized Patient Program coordinator. As with real practitioners, these doctors-to-be must put personal difficulties aside. Regardless of whether students are having a bad day, or if someone cut them off in the parking lot, it all becomes secondary to patients’ needs.

Bill Worthington, a 56-year-old male, unemployed, complains of discomfort in the chest, problems at home.
Jennifer Walsh, a 23-year-old female, in for a routine checkup, exhibits signs of abusive physical injuries.
Anna Smith, a 30-year-old female smoker, presents for shortness of breath and is discouraged after a recent failed attempt to quit.
Fred Johnson, a 70-year-old male, in because his wife says he has trouble remembering things.
Alice McCoy, a 46-year-old female, nervously awaits biopsy results.
Travis Jones, a 16-year-old male, in for evaluation after his mother found text messages about suicide; reports issues at school after coming out as gay.
Sensitive conversations build confidence
“This changed my idea of what it means to learn to be a doctor,” said first-year student Giuseppe D’Amelio. “When we practice on each other, we’re just going through the motions. It’s very different when you don’t know what they (the patients) are going to say.”
Lack of confidence is a common problem, as is talking about highly personal subjects. As first-year student Jared Goodman explains: “Unlike any other conversation you’ve had in your life, you realize that every sensitive detail comes out in the first five minutes.”
From bowel movements to sexual behavior, all topics are open for discussion. “Up until now, social conditioning taught students not to talk about these things,” Glueck said. “They’re not always sure what words to use. That’s where we come in.”
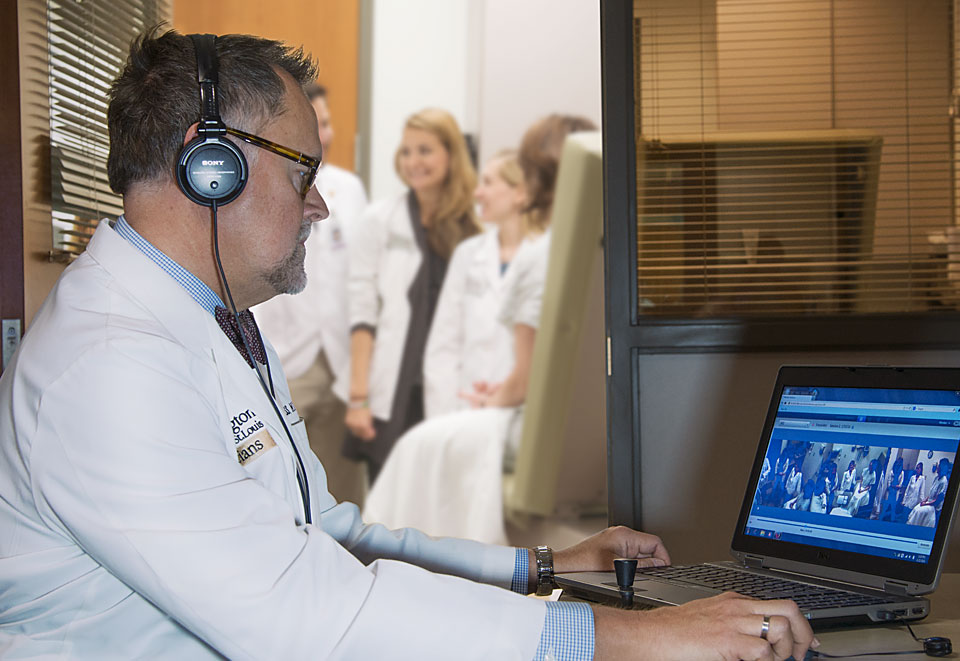
Through video playback, students critically assess themselves, quickly realizing how often they say “um,” fidget, click their pens or look down at the floor. With input from faculty mentors, students go right back in, adjust the approach and try it again. Individualized attention is the program’s hallmark.
In a word, most students describe those early experiences as “terrifying”; many walk into the simulated exam room, nervous and trembling, not exactly sure what to do. Clipboards are dropped. Hand sanitizer squirts across the room. Just a month before, these students were college kids. Now, they must face a patient — albeit, pretend — and appear “doctorly.”
The SPs are ready: They’ve memorized symptoms, medication dosages, family medical history and work-life balance.
Together, Glueck, who enjoys screenwriting, and Pitt, who acts with local and national theater companies, have found their calling. The pair researches and develops a wide range of realistic scripts, complete with backstories, costume and props. Actors are carefully coached and scripts are rehearsed extensively.


Forget about winning Oscars
Despite thoughtful scriptwriting, the actors never know exactly what a student will ask. The job requires intense concentration. At times, SPs are interviewed by up to 10 students in succession.
“It’s not about an Oscar-award-winning performance,” Pitt said. “It’s about a consistent, reliable portrayal of symptoms. In our auditions, we look for people who have experience providing honest, constructive feedback without any medical biases.”
“You had a good demeanor,” five-year SP veteran Aarya Locker told one student. “I think our rapport derailed a bit when I asked you a question and you didn’t know the answer. It’s always fair to say, ‘I don’t know. Let me research that and get back to you.’ I would have been floundering a bit, had I left the office without a solid understanding of the next steps I should take with my child.”
In one small-group session, a student decided his peers were “dancing around the subject too much.” He went into the exam room and flatly told the SP, “You’ve got cancer.” The SP burst into tears.
“The actors respond exactly to what’s in front of them,” Glueck said. “And this dramatically changes what a student can learn. In the student’s second attempt, he gave the diagnosis and met the patient where she was, rather than thinking he knew how it should be done.”
St. Louis’ large professional acting community offers expertise and versatility. “It’s an absolute dream to play someone else and see if it’s believable,” said Reggi, an actor, director and producer who trained at Second City. “I have to step outside of myself, remain neutral and think about how this other person would respond. Certainly, it’s less random than improv, but it still requires spontaneity. It’s where art and science meet.”
Discovering individual styles
Program facilitators design simulated cases that reflect the region’s actual patient population, deriving input from clinical faculty, and building in elements of religious, ethnic and economic diversity. They strive to promote the use of appropriate, inclusive language and create scenarios that may be outside of the students’ comfort zone, such as a same-sex couple seeking treatment for an adopted child.
The students are given a host of increasingly difficult scenarios each year. In their second year, students simulate an evolving physician-patient relationship by visiting the same SP multiple times. Third-year students participate in specialized SP encounters during rotating clerkships.
“The idea is that the more robust you make the practice environment, the more powerful and richer the insights,” Glueck said.
“Students bring innate abilities of varying degrees,” added Alan I. Glass, MD, assistant vice chancellor and director of Habif Health & Wellness Center. As a clinical skills section leader for first- and second-year students, Glass works closely with the SP program.
“For some students, it’s very easy,” Glass said. “For others — like in any subject — it takes more effort. We can teach them skills to be more effective.”
Glueck cautions, however, it’s not about making students all the same. It’s about helping students discover their individual styles so they can communicate in a way that feels natural and genuine.
“Over the course of time, we have a record of multiple patient encounters, and footage of them interacting with different people,” Glueck said. “We use this to see where students are struggling and translate this into actionable steps we can work on together so they can become the kind of doctor they want to be.”
Having gone through the entire SP program, fourth-year student Phillip McGuiness feels he is ready to face the real thing. “Much of the mental acrobatics, the awkwardness, is gone. The standardized patients just take it all in stride. These professionals have played a big part in making me a more efficient, compassionate doctor.”
For many medical school alumni, fellow classmates were the first “standardized patients.”
“We learned physical exam skills on each other,” said Alison J. Whelan, MD, senior associate dean for education at the medical school. “There was no instruction on communication. Over time, the medical community has realized that body language does matter — how you sit, how you look at a patient, how you acknowledge what they are saying.”
Nationally, medical schools are paying more attention to so-called “soft” skills and adding standardized patient programs into their curriculums.
In 2004, the National Board of Medical Examiners added the Step 2 Clinical Skills component, a pass/fail test that is one of three steps students must complete before applying for a medical license.
In Step 2, fourth-year medical students travel to a testing center and assess 12 standardized patients over eight hours, with 15 minutes for each encounter and 10 minutes to record each patient note.
Prior to taking Step 2, Washington University requires students to complete an in-house Clinical Competency Exam — in which they must evaluate six standardized patients in a day. Not all medical schools offer this preparatory advantage for Step 2, the results of which factor into the residency match.
“The Washington University directors have developed novel approaches that serve as a fantastic model for those of us around the country teaching communication skills to our students,” said Lisa Bernstein, MD, FACP, associate professor of medicine and director of Becoming a Doctor curriculum at Emory University School of Medicine. Bernstein also served on an NBME communication skills task force.






