O.R. prep
Surgery’s seismic shift from time- to competency-based training
By Deb Parker
Learn More
Video of the Top Gun competition
Residents win national quiz competition
General surgery residency at Washington University School of Medicine
For 100 years, general surgeons have learned their craft in exactly the same way. As residents, they spent most of their waking (and non-waking) hours in the hospital, shadowing more experienced surgeons and jockeying for time in the O.R. There was no academic curriculum per se; the patient mix dictated the day’s lesson plan. The “apprentice” model has remained largely unchanged.
This broad-based surgical field and its proliferation of increasingly sophisticated tools and techniques — combined with a U.S. mandate for reduced residency training hours — is making learning by osmosis all the more challenging. The ever-expanding body of knowledge is staggering; the time to learn it has shrunk.
As a result, nationally, general surgical education is in the midst of transformation. “The next five years will look nothing like the last 50,” explained Michael M. Awad, MD, PhD, assistant professor of surgery and associate dean for medical student education.
At the institutional and national levels, Washington University educators are devising improved methods to teach surgical skills. Consistently, School of Medicine faculty members have been ahead of the curve in surgical education — crafting a curriculum, employing skills labs outside the O.R., implementing quantitative evaluation measures and designing customized experiences for residents.
Nationally, schools are moving away from
“one-size-fits-all” programs, instead customizing for individual aspirations.
Fewer training hours
A number of factors over the past 10 to 15 years have altered the training landscape. Declining clinical reimbursements require doctors to see more patients to make the bottom line, allowing less time to teach. And residents are spending much less time in the hospital.
In 2003, the Accreditation Council for Graduate Medical Education (ACGME) limited the resident workweek to 80 hours. This mandate, a response to patient advocacy groups, was an effort to reduce medical errors.
“Now that residents are in the hospital less, the ‘education-by-accident’ model doesn’t work as well,” Awad said. “We have to do education by intention.”
The reduction affects all medical residents, but surgical training programs, in particular, had difficulty making the switch. Research indicates a strong link between a surgeon’s operative skill, the number of operations performed and patient outcomes.
“Resident graduates today voice a concern about their lack of preparedness for independence,” said Timothy J. Eberlein, MD, chair of the Department of Surgery and surgeon-in-chief at Barnes-Jewish Hospital. “Not long after the introduction of an 80-hour workweek, there was a national increase in the percent of residents failing the certifying examination of the American Board of Surgery.”
Due to medicolegal concerns, the ACGME restrictions tightened again in 2010, calling for greater supervision of physicians-in-training. Interns now must be directly supervised when performing a critical portion of any procedure.
In the past, surgical trainees became increasingly autonomous during residency, gaining the necessary expertise for independent practice. “Before, you could do five years of residency and hang your shingle,” Awad explained.
Today, however, most aspiring general surgeons undertake one to three years of post-residency fellowship training to strengthen skills and specialize.
General gets specialized
“General surgery” and “specialization” might seem like a contradiction in terms, but the field’s scope is so wide, it’s virtually impossible to master all aspects.
General surgery encompasses the abdomen, breast, skin and soft tissue, the endocrine system, transplants, pediatric surgery, critical care, surgical oncology (including head and neck surgery), emergency surgery, the alimentary tract (including bariatric surgery) and vascular surgery.
“The public also drives the push for specialization,” Awad said. “If you’re getting your hiatal hernia repaired, do you want to go to someone who does two or three a year, along with thyroid and gallbladder procedures, or do you want to go to someone who does 100 of these operations a year?”
Additional, specialized training time is needed, according to a 2013 study in the Annals of Surgery. Awad partnered on the multi-institutional study in which U.S. fellowship directors assessed the preparedness of general surgery residents after completing nine years of training (medical school and residency).
The result: 30 percent of fellowship directors felt that those entering fellowship could not independently perform a gallbladder removal, 19 percent felt that incoming fellows could not sufficiently operate laparoscopic tools and 56 percent felt they could not perform laparoscopic suture techniques.

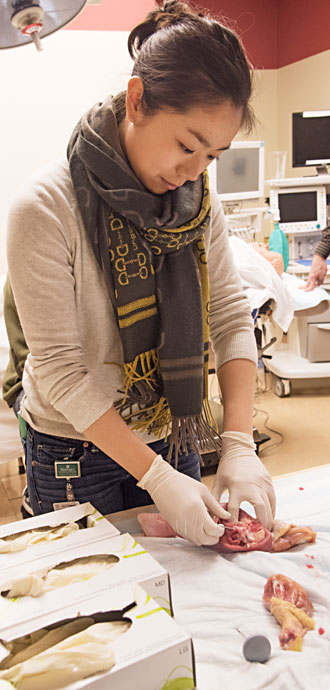
Technology revolution
These percentages perhaps further underscore the breadth of general surgery and the dizzying array of laparoscopic, endovascular and robotic techniques.
The push for better patient outcomes has fostered ever-more-minimally invasive procedures. There used to be one way to remove a gallbladder — through a five-inch abdominal incision; now there are at least three ways.
At a recent Washington University Mini-Medical School session geared for the general public, audience members gasped in unison as they watched a video of a surgeon removing an appendix — through the patient’s mouth.
By passing surgical instruments and a tiny camera through a natural opening in the body, the surgeon is able to perform incisionless procedures.
However, it’s not entirely out-with-the-old and in-with-the new. Surgeons must be prepared to operate the old-fashioned way if complications develop, despite less practice with these procedures.
Critical shortage
The complexity and added debt and training time have made general surgery a less attractive career option for medical students, who may prefer to match to a non-surgical specialty right out of school. “The average medical student is no longer the single male who spends 168 hours a week at the hospital,” Awad said. “People want a life and families. Arguably, that makes for a more well-rounded person and doctor.”
In 2003, general surgery nationally had a number of unfilled residency positions in the Main Residency Match; this, combined with unfilled spots in 2002, served as a wake-up call. The country continues to face a general surgeon shortage, particularly in rural areas. Almost half of U.S. counties have no general surgeons.
“It was of concern,” said Mary E. Klingensmith, MD, the Department of Surgery’s vice chair for education and the Mary Culver Distinguished Professor of Surgery.
“We realized that change was needed to bring the best and brightest to our field to ensure a stable workforce for the future.”
Time for change
Anticipating many of these pressures, Washington University leaders have been retooling the training regimen and implemented an 80-hour workweek at the medical school before the mandate.
“The ACGME adjusts its rules frequently, often giving advance notice of planned changes,” explained Paul Wise, MD, general surgery residency program director. “Here, we use ‘future’ regulations as our guide. We are a very proactive, progressive, almost risk-taking program as opposed to many more conservative programs that wait to let others sort out what will and won’t work.”
With prototype programs in place, the medical school is well poised to lead the national discussion about how best to train future surgeons. Klingensmith directs a consortium of eight U.S. surgical organizations, known as SCORE, which collaborate to develop a unified training curriculum, something that previously did not exist.
The web-based curriculum is updated annually. “We look at the technological advances and ask, ‘Is that a standard we want to make sure every resident is learning?’” Klingensmith explained.
Nearly two decades ago, Klingensmith, a fledgling resident herself, observed as the attending physician performed a mastectomy. Suddenly, the attending turned to Klingensmith and said, “OK. Close it up,” before promptly exiting the room.
“As I looked down at this young patient, I thought, ‘You’ve got to be kidding me. I’m learning right now,’” Klingensmith recalled. “I felt enormous pressure to make the incision look as nice as I could. I thought if I’m ever in a position to change surgical education, I’m going to do something about this.”
Gaining proficiency
Klingensmith, who began directing the general surgery residency at Washington University in 2001, made good on her promise, developing a skills training lab outside the O.R. that would expose residents to graduated levels of experience and provide practice opportunities in a low-stress environment.
A novel concept at the time, only two other institutions offered such labs: Southern Illinois University-Springfield and the University of Toronto.
Washington University has made major investments in the lab, formally the WUSM Institute for Surgical Education, accredited as a Level 1 (top) institute by the American College of Surgeons in 2012. Awad, nurse coordinator Debbie Tiemann, RN, and surgical technician Angelia DeClue, RST, now administer the lab.
Tools range from low-tech plastic body parts to highly realistic computer simulators. Students and residents can remove a virtual gallbladder before ever putting scalpel to flesh. Laparoscopic box trainers test precision and speed as residents transfer rows of pegs using a video monitor as a guide. Trainees also perform progressively challenging procedures in animal models and human cadavers.
“There isn’t any question that working on fundamental skills translates to the operating room,” said L. Michael Brunt, MD, professor of surgery and chief of the Section of Minimally Invasive Surgery and president of the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES).
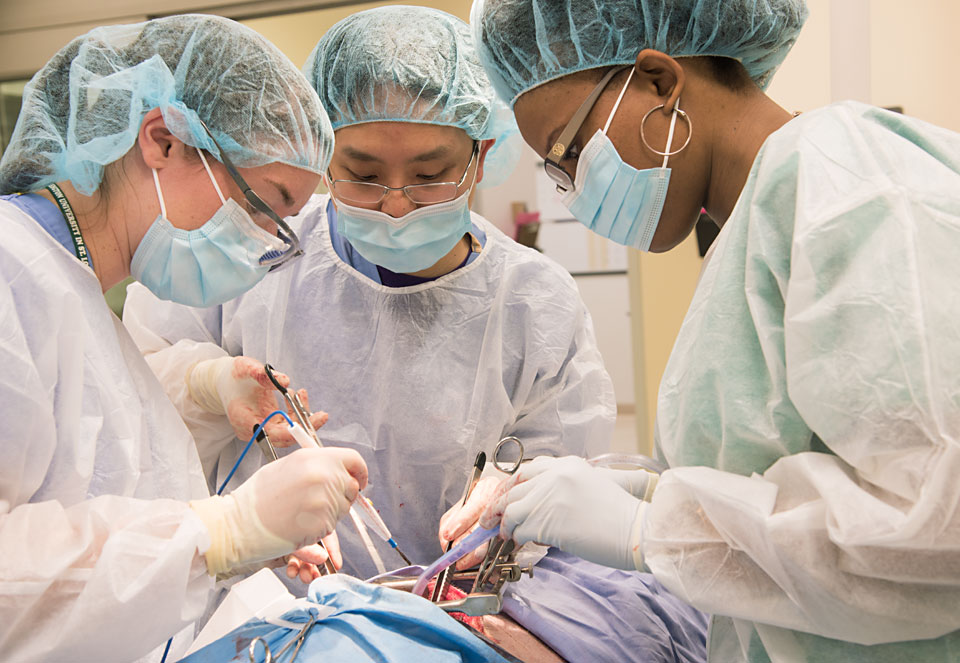
“The academy model has revolutionized my education. I have witnessed that I can achieve the same competencies much more quickly in this streamlined and personalized approach.”
ASHLEY M. HOLDER, MD
Individual experience
Traditionally, surgical residents have received little formalized performance feedback. Washington University is piloting an “academy model” that outlines core competencies and key milestones for several general surgery sections. “We are moving toward competency-based rather than time-based training,” Awad said.
The model stipulates that residents discuss learning objectives with faculty as they begin a rotation, receive mid-term feedback and undergo formal assessment at the end.
To more accurately gauge trainee performance, input is collected from nurses and technicians, as well as faculty. Awad then meets personally with the resident. If a resident is struggling in a particular area, he or she is paired up with a senior resident for as long as it takes to refine the skill.
“The academy model has revolutionized my education,” said fifth-year surgical resident Ashley M. Holder, MD, who began training at the medical school before the model was introduced. “I have witnessed that I can achieve the same competencies much more quickly in this streamlined and personalized approach.”
Another significant change nationally is a shift away from “one-size-fits-all” programs requiring residents to complete identical training modules across five years.
“As medical care becomes increasingly complex, it’s evident that not every individual needs to learn the entire breadth of surgery,” Klingensmith said. “For instance, do trainees going into heart surgery ever need to do pancreas surgery? Right now, that is a requirement. But it may not make a lot of sense in the big picture.”
Customizing residency training to individual aspirations could maximize the experience — reinforcing select skill sets while decreasing the dependency on fellowships.
Klingensmith is leading a nine-institution consortium examining flexibility in surgical training. At participating institutions, residents in their third, fourth or fifth years may spend 12 months in specialized rotations that will better prepare them for their intended areas of practice. The institutions are evaluating the effectiveness of such a model and collecting data on resident performance.
Washington University’s general surgery residency was one of the earliest to develop a “fast track” in cardiothoracic (2005) and vascular (2006) surgery, allowing senior residents to focus on these areas. The vascular surgery section took it a step further in 2013; trainees do not enter a general surgery residency, but rather spend five years learning vascular surgery almost exclusively, with some general surgical skills taught early in the program.
“Training the next generation of surgeons will require the types of programs we are developing, which are intentional, structured, rigorous and customized,” Awad said. “We no longer can rely on whatever happens to come through the operating room doors.”






