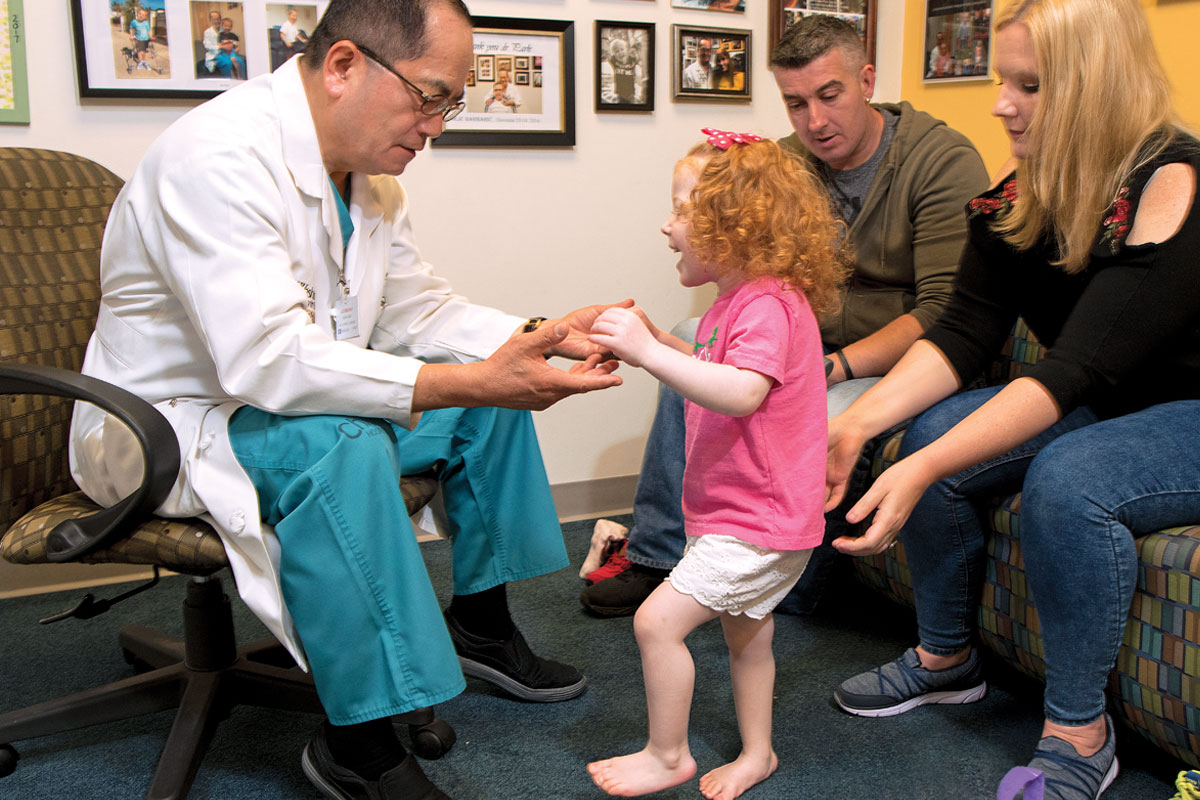
As a baby, Alexa Reed seemed to be hitting all her developmental milestones. When it came time to walk, however, she started having trouble. Her right foot turned inward and she had a tendency to rise up on her tiptoes.
“For two years I asked her pediatrician if this was normal and if I should do something to fix it,” said Amy, Alexa’s mom. “We were told that she would grow out of it and that no intervention was needed aside from reminding her to walk flat-footed.”
Over time, Alexa’s muscles got tighter, she fell down frequently and increasingly relied on toe-walking. Wearing braces for several years and undergoing weekly physical therapy to stretch her tight legs did not improve the situation.
At nearly 4 years of age, Alexa finally received a definitive diagnosis: spastic diplegic cerebral palsy (CP), a chronic neuromuscular disorder that causes tightness and spasms in the extremities. Most commonly caused by lack of oxygen and early damage to the brain, spastic CP accounts for almost 80 percent of CP cases.
Soon after Alexa’s diagnosis, the Reeds moved from Los Angeles to St. Louis for a new job and to be closer to family — not realizing that Washington University Medical Campus is home to T.S. Park, MD, a world-renowned, uniquely qualified pediatric neurosurgeon who specializes in treating spastic CP.
Post-surgery, Alexa, now 9, has full function and enjoys hiking, soccer and hanging out with friends. In Alexa and in thousands of other kids worldwide, Park has restored the ability to walk.
Not your average neurosurgeon

Park, the Shi H. Huang professor of neurosurgery, is a pioneer in the use of selective dorsal rhizotomy (SDR), a spinal surgery that he performs at St. Louis Children’s Hospital. In the procedure, Park severs the nerves that cause spasticity. Park has been performing SDR for 30 years, treating more than 3,700 patients from 47 states and 73 countries. Of those cases, only nine have ever required readmission (four for wound infections, five with spinal fluid leaks). Amy found out about Park from an in-home physical therapist.
“It was glaringly clear that our move from Los Angeles back home to St. Louis was somewhat serendipitous,” Amy said. “We were exactly where we needed to be to have the most skilled and successful surgeon on the planet be the one to end the grasp that spasticity had on our daughter for good, and give her a future we had only dreamed of.”
Born in Bristol, U.K., Esme, or Ezzy (as she likes to be called) Hodge, had to come a bit farther for help. Ezzy’s parents noticed their baby daughter wouldn’t reach up for a cuddle and had trouble balancing independently. An MRI at age 2 revealed Ezzy had suffered a brain injury during birth. Like Alexa, she was diagnosed with spastic diplegic CP.
“We were told she would never walk,” said Ezzy’s mom, Angela. “As parents we were truly devastated.”
Angela found Park’s name during an online search for potential treatments. “I knew then I would do whatever it took to get Ezzy this amazing surgery and prayed Dr. Park would say yes to helping our little girl, as he was her only chance,” Angela said.
In the initial patient evaluation, Park’s team tells the family what type of outcome to expect: Will the child walk independently, or with crutches or a walker? Will the child be able to run and jump?
“I’m fairly sure we are the only ones who can give such a precise prediction,” Park said. “Our prediction rate is very high — 85 percent correct.”
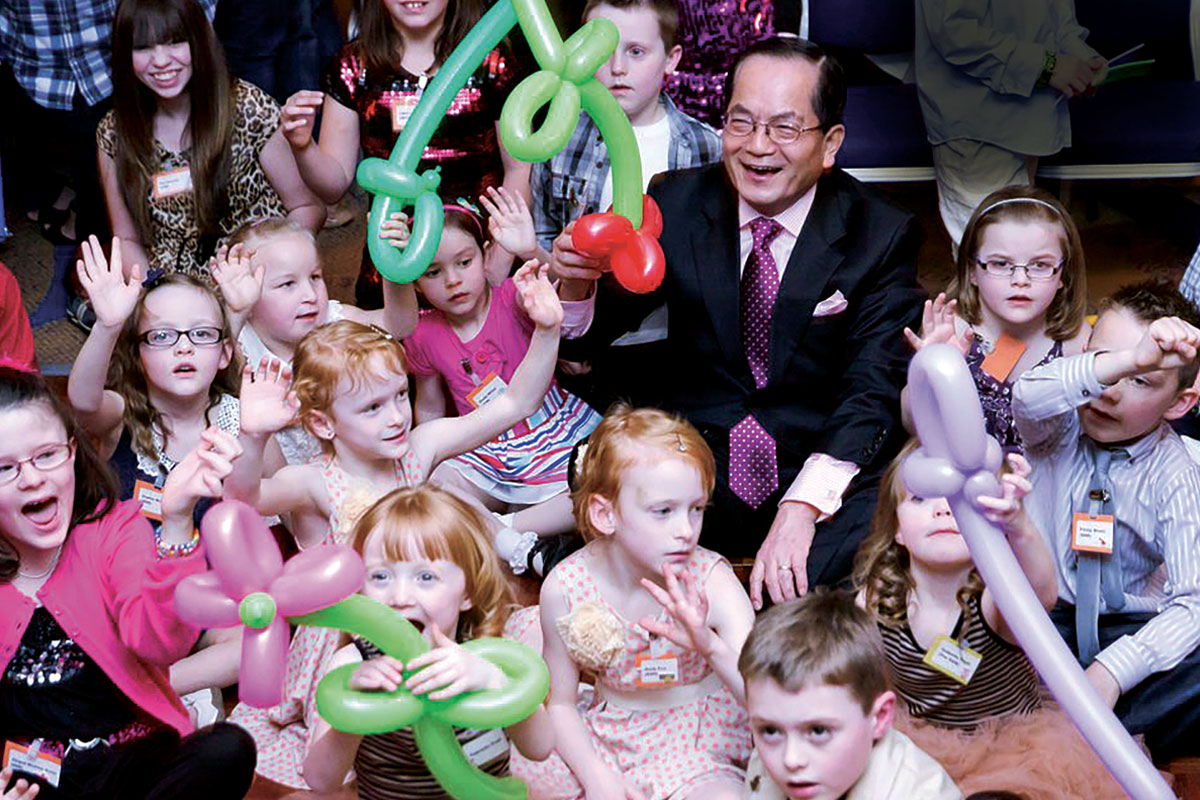
Constantly seeking improvements
Severing spinal nerves that cause spasticity has been going on since the 1900s. But SDR did not make its way to the U.S. until 1986. Once Park learned about it in 1987, he began using the technique. By 1991, he made some key improvements.
The procedure originally involved cutting through five to six vertebrae in the lower spine to access the nerves causing spasticity. Park refined the process so he only needed to cut one lower vertebra. This less invasive method causes no long-term spinal problems and allows Park to perform the surgery on children as young as 2, who heal quickly, as well as patients as old as 50, whose spines would otherwise never heal completely.
Though Park performs the bulk of SDR surgeries on children, he also has operated on 130 adults — more than any other doctor in the world — at Barnes-Jewish Hospital.
Neurosurgeons from across the globe come to observe his surgical methods and techniques. And Park trains fellows at Children’s Hospital in the procedure.
Park also has published nearly 40 papers about the surgery in scientific journals. Because his team is the only one that has performed SDR surgery for three decades, it is in a unique position to study long-term outcomes.
Just this year, Park and his colleagues published two papers: In one, they followed 95 patients between the ages of 23 and 37 who had SDR surgery 20 to 28 years ago, and, in another, they surveyed 294 adult patients who had received SDR surgery as children. Both studies showed overwhelmingly positive results. The improvements these patients experienced in walking and in general quality of life after SDR surgery extended through adulthood and they reported no long-term side effects.
“We can clearly say SDR surgery is the only treatment that can remove spasticity permanently. No other treatment can do this,” Park said.
“He developed — really single-handedly — the operation of selective dorsal rhizotomy for cerebral palsy,” said Ralph Dacey, MD, the chair of neurologic surgery, in a 2017 tribute video honoring Park. “And not only did he develop the processes around doing that procedure very effectively and safely, but he was able to prove its efficacy in a series of papers that have become landmark studies.”
Results “like magic”
The SDR surgery typically lasts three to four hours, followed by a five-day hospital stay. Then, the tough rehabilitation work begins. This includes daily physical therapy with Children’s Hospital therapists. Out-of-country patients like Ezzy are expected to stay in St. Louis for about a month and then they must continue intensive physical therapy at home for a few more months while Park follows the progress remotely.
Ezzy’s improvements began almost immediately after surgery.
“Like magic before our eyes, she made daily improvements,” Angela said this past October. “In just two short weeks, she has managed to walk with a cane, something I wouldn’t have believed unless I saw it with my own eyes.”
Some children, such as Alexa, need an additional orthopedic surgery to lengthen their muscles and/or tendons, which shorten from prolonged disuse.
Park refers these patients to pediatric orthopedic surgeon Matthew Dobbs, MD, who has developed a minimally invasive muscle- and tendon-lengthening surgery that further improves patients’ range of motion and mobility.
The combined surgeries offer dramatic improvements in patients with severely impaired mobility, Park said.
Five months post-op, Alexa started playing sports like soccer and even participated in a 5K race. Nine months after Alexa’s surgery, Amy reported: “Dr. Park joyfully told my daughter, ‘You never have to see my face again!’ She was released from physical therapy and allowed to simply be a kid.”
A global impact
To help spread the word about the life-changing surgery, in 2010, Park and his team started the Selective Dorsal Rhizotomy-St. Louis Children’s Hospital Facebook page. It has since amassed 9,000 followers. Before long, family-run Facebook pages championing Park’s expertise began cropping up — in Brazil, Korea and dozens of other countries.
Park checks the Children’s Hospital and country-specific Facebook pages multiple times a day, replying to questions, posting comments, medical literature and information to help parents and patients navigate the complex world of CP.
Park dedicates time every year to travel the world and examine children with CP to see whether they qualify for SDR surgery. To consult with these patients, he visits hospitals, clinics, sometimes even hotels, like the one owned by his brother in Korea.
Park also tirelessly advocates for health insurance policies to cover the surgery. He’s given talks, for example, in Hungary to the country’s national health insurance program director, and even testified to a British parliament member.
To help make the surgery financially accessible, especially for international families, Park lobbied Children’s Hospital to set a fixed rate of $40,000 for any patient paying out of pocket. Because of his undeniably positive outcomes, the hospital agreed. While many families must spend months or years fundraising for the surgery, this fixed rate provides peace of mind. Park does his part by charging only $100 for initial consults and nothing for follow-up visits.
Motivated by his international patient base, Park also worked to improve the hospital’s interpreter service — something that benefits every non-English-speaking patient who comes through the doors.
Beyond grateful
“At the end of the day I know T.S. Park is what we call a guardian of childhood,” said Joan Magruder, St. Louis Children’s Hospital president, in a 2017 tribute video honoring Park. “He has done everything imaginable to make sure that every child has the opportunity to be a child and to live their childhood to the absolute maximum.”
This year, Missouri Gov. Eric Greitens and St. Louis Mayor Lyda Krewson declared Sept. 9 as Dr. T.S. Park Day. The day was marked by a symposium in Park’s honor.
Families from every corner of the globe make videos showing their children’s growth and progress and regularly post them on the SDR Facebook page — something Park said he loves to see. “I’ve befriended a number of parents,” Park said. “We have personally become very connected.”
It’s a bond that Amy, and thousands of parents like her, acknowledge with gratitude. “The possibilities for Alexa are endless now,” Amy said. “My daughter will live a full healthy life, free from spasticity, thanks to Dr. Park. He is our hero and will be family to us for life.”
Published in the Winter 2017/2018 issue





 Share
Share Tweet
Tweet Email
Email