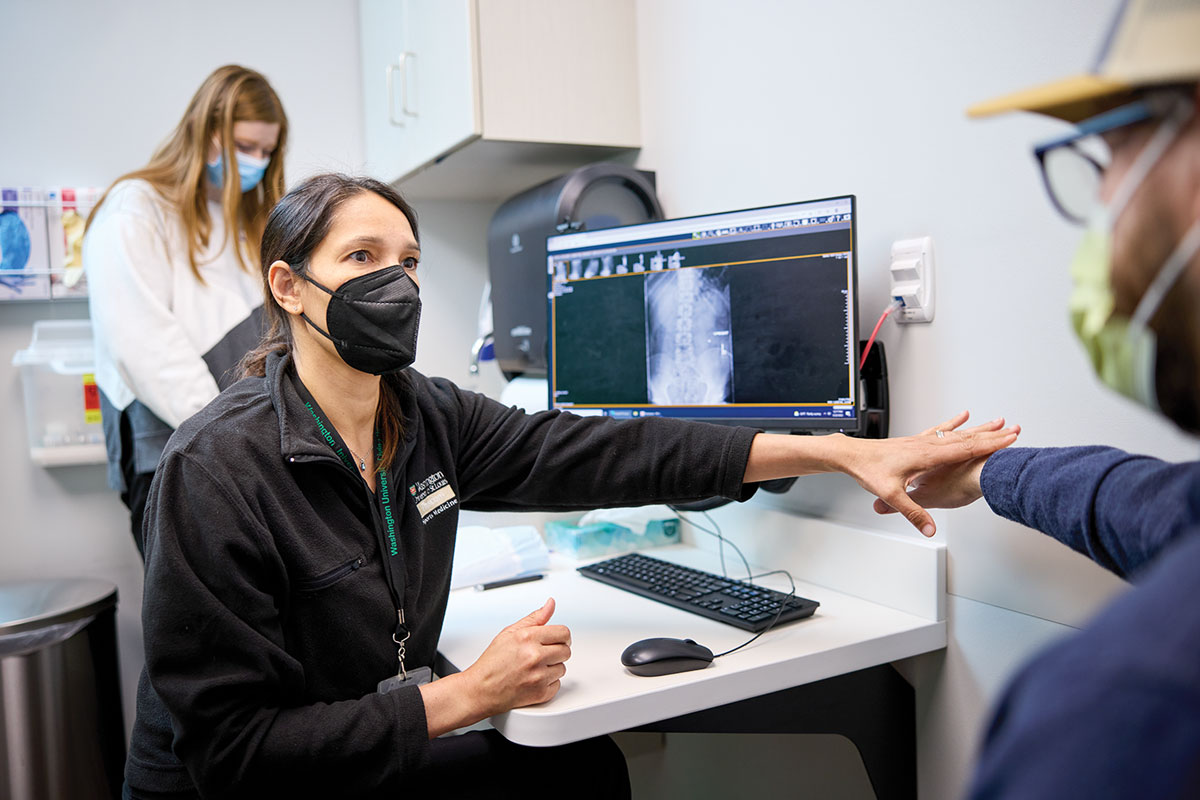
Zach Wood was in the Emergency Department with excruciating lower back pain. After imaging tests, he was sent to see a hip surgeon. Later, the hip surgeon suggested that before advancing to surgery, Wood might consider a visit to the Living Well Center at Washington University School of Medicine. Clinicians at the center could improve the likelihood that surgery would go well, the surgeon said.
Now a regular visitor to the Living Well Center, Wood receives physical therapy, medical massage, dietary counseling and other services. All of that has improved his overall health and reduced his pain. Many months after his first visit, he’s beginning to think he may not need surgery after all.
The Living Well Center provides what’s known as lifestyle medicine. This developing field addresses the root causes of medical problems by focusing on lifestyle choices affecting patients’ health. Using evidence-based techniques, lifestyle medicine practitioners help people change their behavior in ways that might prevent, treat or even reverse cardiovascular disease, Type 2 diabetes, obesity and other chronic conditions.
A good number of lifestyle-focused centers have popped up around the country, but the Living Well Center is different from most because its primary focus is in treating issues that underlie musculoskeletal health.
Wood’s case isn’t typical, in that some of his problems stem from a rare autoimmune disorder, Mixed Connective Tissue Disease. This disorder causes the body’s connective tissue, called fascia, to swell and thicken. Wood’s fascia gets extremely tight, contributing to pain in his back and hip, as well as other issues, including difficulty swallowing.
In response, Living Well Center team members developed a multipronged, targeted approach — involving treatments and lifestyle modifications — to help alleviate inflammation and stress on his body.
“Initially, I thought I was coming to the center as a way to prepare my body for an operation,” Wood said. “Now I feel like what’s happening here is becoming more preventative. The treatments I’m receiving might mean I won’t need to have surgery.”
A lofty vision
Almost a decade ago, Heidi Prather, DO, a former orthopedics professor at the School of Medicine, began to think about creating a clinical center where patients could get their blood sugar under control, lose weight, stop smoking and take other actions to improve the odds that orthopedic treatments, such as joint-replacement surgery, would be successful.
“As clinicians, we know that if you allow patients to become active participants in their own health care, regardless of what the problem is, they do better,” Prather said.
“With the center, we have this lofty goal that patients will come to us needing, say, a knee replacement and, in addition to doing what we can to make the surgery successful, our work will result in better overall health by controlling diabetes or reducing stress, for example — just minimizing some of the problems that contribute to poor health and maximizing the behaviors that improve well-being,” she added.

It took years to develop the center’s strategy and infrastructure, but now patients flock to a suite of offices and exam rooms in one of the new medical buildings on the campus of Barnes-Jewish West County Hospital. The Living Well Center has treated more than 800 patients since it officially opened its doors in 2020, focusing primarily on four groups: candidates for musculoskeletal surgery; COVID-19 long-haulers (particularly those with fatigue and joint pain); those who want to optimize overall health; and cancer survivors. Integrated therapies can reduce the fatigue, nausea, pain, anxiety and other symptoms associated with cancer and cancer treatment.
“All of us went into medicine to help people, but it can be frustrating when, as a provider, you’re unable to change some of the underlying issues that are barriers to your patient’s success. Lifestyle medicine can give you the tools.”
Devyani M. Hunt, MD, a professor of orthopedic surgery, now serves as the medical director of the Living Well Center. Her subspecialty is physical medicine and rehabilitation, also known as physiatry, which applies nonsurgical treatment to musculoskeletal conditions.
“We’re very accustomed to looking at the body and how it all works together,” Hunt said. “I’m always thinking about how the hip is affecting the spine or the knee or the foot.
“Our goal really is to treat the whole patient, and with this comprehensive model, we’re demonstrating that we can improve outcomes for surgery patients and help others avoid surgery, and we can do it all in one place,” she added. “All of us went into medicine to help people, but it can be frustrating when, as a provider, you’re unable to change some of the underlying issues that are barriers to your patient’s success. Lifestyle medicine can give you the tools.”
The health professionals at the Living Well Center come from a variety of specialties. Some, like Hunt, trained in physiatry. Other specialists include a dietitian, psychologist, rehabilitation counselor, massage therapist, acupuncturist, physical therapists and a physician assistant.
Hunt said the specialists at the center work together to apply the “pillars” of lifestyle medicine. These include using food as medicine by teaching a diet consisting mainly of plant-based foods; encouraging physical activity and exercise; addressing sleep issues; managing stress and addressing anxiety and depression — problems often encountered by people who are in pain; avoiding risky substances, such as tobacco; and encouraging positive social connections.
“One goal is to provide our patients with health care, rather than sick care,” Hunt explained.
Walking into the Living Well Center is like walking into any other clinical office in some ways, but if visitors are paying attention, they’ll notice the waiting room lights aren’t quite as bright or intense as in many doctors’ offices. Plus, along with soft music, it’s also possible to hear the chirping of songbirds coming through the speakers in the waiting area. “Part of our focus is on managing stress,” Hunt said. “That’s why we’ve tried to make a beautiful respite for patients.”

Just down the hallway is a teaching kitchen and gathering area where patients learn to cook healthier foods. Registered dietitian Nartana N. Mehta helps people improve their diets using one-on-one counseling, cooking classes and demonstrations.
“Every person is unique, and their eating plans should reflect that,” Mehta said. “We know that certain foods can contribute to inflammation while other foods can reduce it. Still other foods can help keep blood glucose levels under control. Our goal is to help people get healthier by increasing their consumption of plant foods like fruits and vegetables, whole grains and legumes to try to reduce levels of inflammation because we know that less inflammation can mean less pain.”
The gathering area doubles as a community space for patients to have shared medical appointments, take group yoga or Tai chi classes. “We want patients to experience these things together because the literature tells us that if we don’t do certain activities as a community, it doesn’t really sink in, and people can’t move forward as successfully,” Hunt said.
Obesity and aging
The Living Well Center is stepping into a rapidly expanding area, as the medical community today contends with a global obesity epidemic. Obesity has a significant impact on the musculoskeletal system and is associated with both degenerative and inflammatory conditions. It is the leading preventable cause of wear-and-tear arthritis, known as osteoarthritis.
More than 800,000 people have their knees replaced each year in the U.S., with another 450,000 hip-replacement surgeries annually. In addition, some 65 million Americans report a recent episode of back pain, with about 16 million — 8% of all adults — reporting that they suffer persistent or chronic back pain. As the population ages, these numbers are continuing to trend upward.
Being overweight increases the need for joint replacement and worsens surgical complications, resulting in higher rates of infection, blood clots, component failure and dislocation. In addition, overweight people are more likely to have diabetes, a condition that complicates wound healing, another concern when considering surgery.
People who smoke or whose blood sugar isn’t well-controlled also are at risk for health issues following joint-replacement surgery. In fact, many in need of new hips or knees are told that they first must lose weight, better control their blood sugar or quit smoking.
That’s frustrating for patients who are in pain, but it’s also frustrating for doctors when patients’ lifestyles make surgical outcomes less predictable. Hunt explained that with so many different types of health professionals under one roof, the center is able to personalize treatments and offer evidence-based therapies to improve surgical outcomes.
“If a patient comes in with a goal of getting their body ready for a hip replacement, but isn’t able to do that because their blood sugars are not well-controlled or their BMI is too high, they’ll find that we have some tools we can use to change that,” Hunt said. “We can prepare them in ways that lower their chance for infection after surgery and reduce the odds that they’ll need to come back to the hospital with a complication.”
Genny Watkins had hoped to lose a little weight before having a complicated surgery on her lower leg that involved stabilizing her ankle and lengthening her Achilles tendon. Her surgeon, Jonathon D. Backus, MD, an assistant professor of orthopedic surgery, recommended she visit the Living Well Center in the months before her operation.
In addition to excess weight, Watkins had other underlying conditions, including an incomplete spinal cord injury. She knew that being immobilized and unable to walk for several months following surgery likely would cause her stress, so during visits to the Living Well Center, she focused on changing her diet and getting behavioral health support.
“My body mass index went down and I lost 12 pounds,” Watkins said. “I also took a Zoom class on behavior modification, and Mollie Semmer (physician assistant) helped me find a good physical therapist and psychologist. The Living Well Center team really got me prepared for a very challenging surgery.”
The center also offers massage therapy, physical therapy and acupuncture to treat pain.
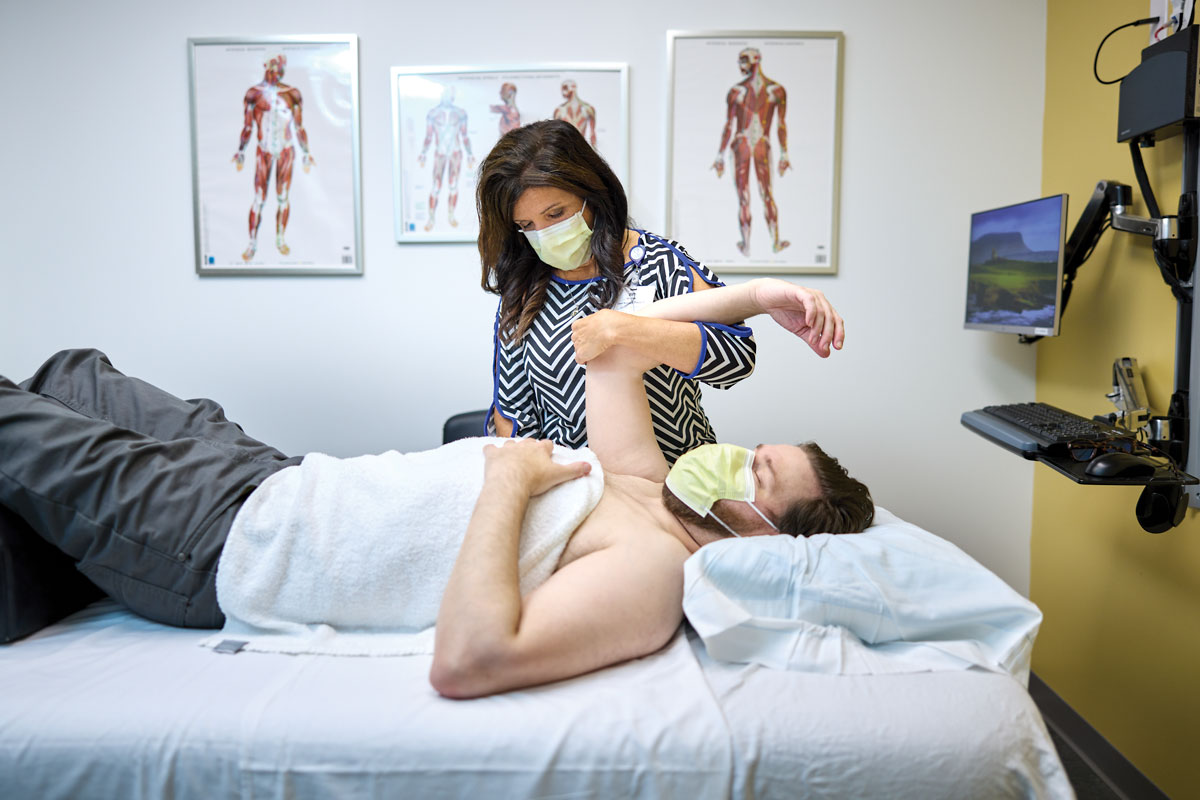
“Acupuncture is less invasive and has fewer side effects than many other pain treatments,” said Chi-Tsai Tang, MD, an associate professor of orthopedic surgery, who trained as a physiatrist and later studied acupuncture with physicians in China. “It’s a perfect complement to my physical medicine and rehabilitation training.
“Acupuncture works through various means, the main one being to release myofascial tension. It can also work through the endogenous opioid system, causing the body to release its own pain-inhibiting substances, like endorphins,” he added. “It also has been shown to cause changes in parts of the brain that are involved in the processing of pain.”
Tang explained that acupuncture often works because the various parts of the body are linked and operate together. Those types of connections underlie many of the treatments offered at the center. Diet, for example, not only affects the gastrointestinal tract, but through gut-brain connections, it also can affect mood and pain perception. Stress can increase tension and contribute to pain.
In centers that treat people with diabetes and cardiovascular disease, it’s relatively common to offer stress management, smoking cessation and diet modification. Although it’s well-established that those same issues can exacerbate musculoskeletal pain, very few centers have embraced lifestyle medicine in the treatment of musculoskeletal problems. Part of the reason is that although the links between diet and problems such as heart disease and diabetes are widely accepted, there’s not as much attention paid to the links between diet and pain in the knee or the hip.
As the center employs lifestyle medicine strategies not normally seen in an orthopedics practice, doctors there are rigorously testing its strategies.
Abby L. Cheng, MD, an assistant professor of orthopedic surgery, studies patients who come through the center’s doors and compares their results to those of patients treated using standard care models. Living Well Center patients are more likely to have diabetes or obesity than those who receive standard care, she has found. They’re also more likely to have exhausted other treatment options available to them.
But the Living Well Center now has empowered many such patients, like Zach Wood and Genny Watkins, to navigate through these complex issues and achieve significantly improved health.
“Everything in my daily life has changed for the better,” Wood said.

Showcasing success: Patient overhauls health
David Capes is a local attorney, avid travel photographer and golfer. He also has suffered chronic back pain from arthritis, disc degeneration and diabetic neuropathy. “I had previously always been upbeat about life, but the pain was seriously affecting my attitude and well-being,” he said. Capes connected with the Living Well Center’s Devyani Hunt, MD. She customized a treatment plan involving acupuncture, physical therapy, medical massage, education about pain-diminishing techniques and stress management, and nutrition counseling. Today, Capes walks up to 20 miles a week. Hunt said she knew immediately she wanted to display his work throughout the center: “He captures moments and people in a way that draws you in and takes you to a special place of possibilities. It’s perfect for the Living Well Center.”
Published in the Autumn 2022 issue





 Share
Share Tweet
Tweet Email
Email