
Depression can be diagnosed in children as young as 3, according to a research team headed by Joan L. Luby, MD (left), a professor of child psychiatry and director of the Early Emotional Development Program.
Nearly one in 10 U.S. adults is clinically depressed. Of those, approximately one-third have major depressive disorder, a long-lasting and severe form of the illness. It’s a leading cause of disability for people between the ages of 15 and 44. Even when symptoms subside, problems often recur and can periodically disable a person throughout life.
For many, depression begins in early childhood. That’s one of the major findings from a team of child psychiatrists, psychologists and social workers led by Joan L. Luby, MD, a professor of child psychiatry and director of the School of Medicine’s Early Emotional Development Program. She has spent the better part of her career trying to identify, classify and treat depression in children as young as 3 years of age.
“A primary characteristic of healthy, young preschoolers is that they tend to be inherently joyful,” Luby said. “One of the main symptoms we see in depressed children is anhedonia, which is the inability to experience joy.”
When Luby began her research in the early 1990s, many in the field of child psychiatry didn’t believe preschoolers could be clinically depressed.
Beyond conventional thinking
Some thought it was possible for children to become depressed only as they got older and started school. Others believed that, even if preschoolers could get depression, it would be impossible to diagnose it so early.
But Luby’s team has demonstrated that both of those opinions were wrong. The researchers found by slightly altering some of the diagnostic criteria to more age-appropriate levels, it was possible to identify and diagnose depression in kids as young as 3. Further, the team discovered that children who are depressed as preschoolers are more likely to battle the disorder when they enter primary and middle schools.
Simply figuring out that some very young children suffer from depression isn’t really the goal, however. Early identification and intervention potentially could alter the course of this often chronic, recurrent disorder. Luby would like to make clinical depression a condition that can be treated and overcome.
“It may be possible to shift the developmental trajectory when children are still young and their brain networks are more plastic and able to change and adapt,” she explained.
Luby and her colleagues are studying an approach known as Parent Child Interaction Therapy-Emotion Development (PCIT-ED), based on a type of therapy developed and tested in the 1970s.
Originally, the technique consisted of two parts. First, the parent was encouraged to get down on the child’s level, play games that the child wanted to play, be very enthusiastic and use effective praising techniques. In the second part, parents learned to use discipline strategies, such as “time-outs,” with their children.
Luby’s team created a third component — the emotion development (ED) part of PCIT-ED. Through this, parents are taught to: recognize their children’s emotions; help their children recognize emotions; and guide their children in effectively regulating these emotions.
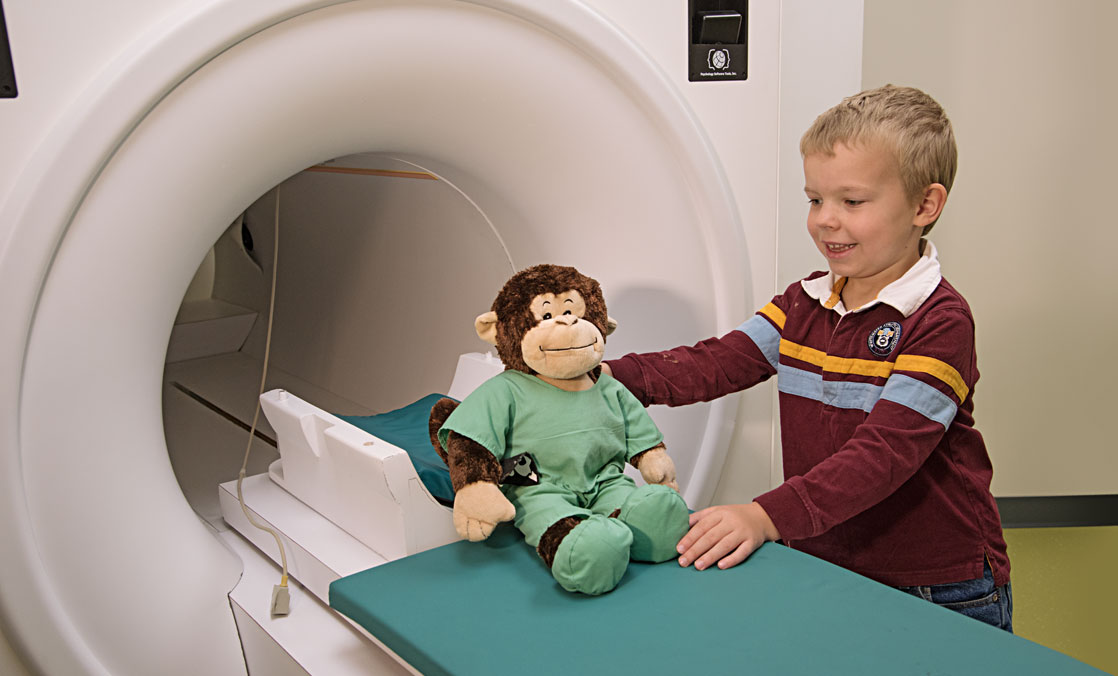
Enclosed scanners are often unnerving for adults, much less these young children who must hold still and perform basic tasks while inside the noisy machines. So the researchers have developed a novel approach. Children undergo “practice scans” first with a device that looks like the real thing, all in a playful environment that helps overcome anxieties.
Intervention shows promise
A pilot study of the technique showed that depression severity scores decreased by 44 percent in preschoolers during an 18-week intervention. At the study’s end, most of the kids who did PCIT-ED with a parent no longer met the diagnostic criteria for clinical depression.
But that was a small study. Now, the researchers are in the middle of a very large trial of the intervention.
One participant is the 5-year-old daughter of a nurse at St. Louis Children’s Hospital. Requesting anonymity, the mother reported that, after 16 weeks of the PCIT-ED intervention, her daughter is doing much better. Previously, her daughter struggled at home and in preschool. Although the problems have not disappeared, they now are less frequent.
“She has cycles of irritability and tantrums, when she doesn’t like to comply with what’s expected of her,” the mother explained. “When we started the study, she cooperated about one-quarter of the time, but now I’d estimate that she actually does comply the vast majority of the time. And through this type of play therapy, we’ve grown closer because we have to sit down every day and work through things together.”
Additionally, the researchers are using MRI to look at brain structure and function; they want to see whether the brains of depressed preschoolers look and act differently than the brains of young children who are not depressed. Also, they want to learn whether therapy changes anything.
“We’re looking for changes in the way the brain is organizing itself across development,” said Deanna Barch, PhD, the Gregory B. Couch Professor of Psychiatry, professor of psychology and of radiology. “That can be related to changes in the structure of the brain, both in gray matter development and white matter connectivity. It also can be seen in how the brain activates when challenged cognitively or emotionally, as well as the ways that different brain regions communicate with one another.”

As parents interact with their children in an observation room, clinicians can offer guidance via an earpiece.
A possible anatomical sign
The team recently published findings from an imaging study of previously depressed school-age kids in the November issue of JAMA Psychiatry. In 145 children who underwent MRI scans between the ages of 6 and 12, the researchers found that a part of the brain called the anterior insula was smaller in the children with a history of preschool-onset depression. The anterior insula is part of the brain’s insular cortex, which is believed to be involved in emotion, perception, self-awareness and cognitive functioning, among other things.
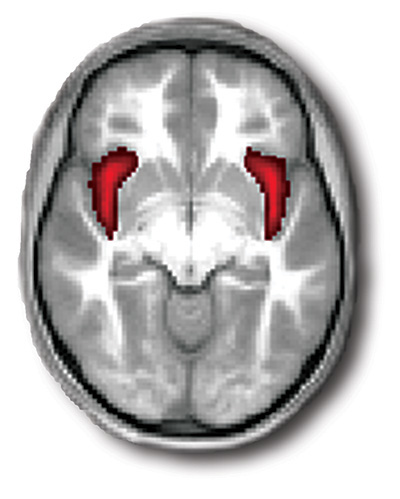
A smaller anterior insula, red, may be linked with childhood depression.
The anterior insula connects directly with the amygdala, another brain structure closely linked to emotion, and one that functions differently in depressed preschoolers, according to research by Michael S. Gaffrey, PhD, assistant professor of psychiatry.
It’s too soon to know whether the smaller anterior insula puts children at risk for depression, or whether the condition affects the brain’s anatomy. Studies by other researchers indicate that smaller insula volumes also are common in depressed adults.
First author Andy C. Belden, PhD, said that “pathological guilt,” a key symptom that commonly accompanies depression, is linked with reductions in anterior insula volumes.
Toddlers who display pathological guilt prior to age 3 are 10 times more likely than their peers to be diagnosed with depression by age 5. Guilt, Belden said, may be a strong marker for depression risk.
“In young children, pathological guilt is like an excessive self-blame for things that kids have — or even haven’t — done,” said Belden, an assistant professor of psychiatry. “Children with pathological guilt tend to apologize, and to genuinely feel bad about very many things, and it interferes with their functioning. The ‘million-dollar question’ is which comes first? Do you have depression and that makes you feel more prone to guilt? Or does a guilt-prone person become depressed?”

Study first author Andy C. Belden, PhD, explains one of the assessment tools. This caplike device makes it easier to measure brain electrical activity in young children.
Earlier could be better
To better assess the impact of early intervention, the researchers also are using electroencephalography (EEG) to measure brain electrical activity while study participants view pleasurable scenes. A caplike device worn on the head makes this easier to use in very young subjects.
By comparing those measurements pre- and post-therapy, it is possible to see whether there are any pattern changes in the electrical activity.
“There are lots of reasons to believe that early intervention is going to be much more effective, not only in treating depression, but also across a wide range of brain-related disorders,” Barch said.
Because depression is common, many people don’t view it as being all that serious, Luby acknowledges. This can make it even harder to take seriously diagnoses in young children who are still incapable of fully regulating emotions. But make no mistake, she said, depression is deadly. It is a factor in about two-thirds of the 30,000 suicides committed yearly in the U.S.
“Only depressed people really understand how bad it is,” she explained. “Even people who have serious pain from cancer don’t necessarily want to kill themselves. Depression presents a whole different type of pain, psychic pain, and its depth and severity isn’t fully appreciated in our society.”
Like childhood cancers, Luby suspects depression that begins early in life often may be more aggressive than forms of the disorder that appear later. If PCIT-ED, or some other therapy, can change the path of the illness, a good deal of disability, psychic pain and even death may be prevented.
Published in the Winter 2014/2015 issue





 Share
Share Tweet
Tweet Email
Email